Uterine Fibroids: Causes, Symptoms & Treatment
Complete guide to understanding uterine fibroids, their symptoms, diagnosis, and comprehensive treatment options.
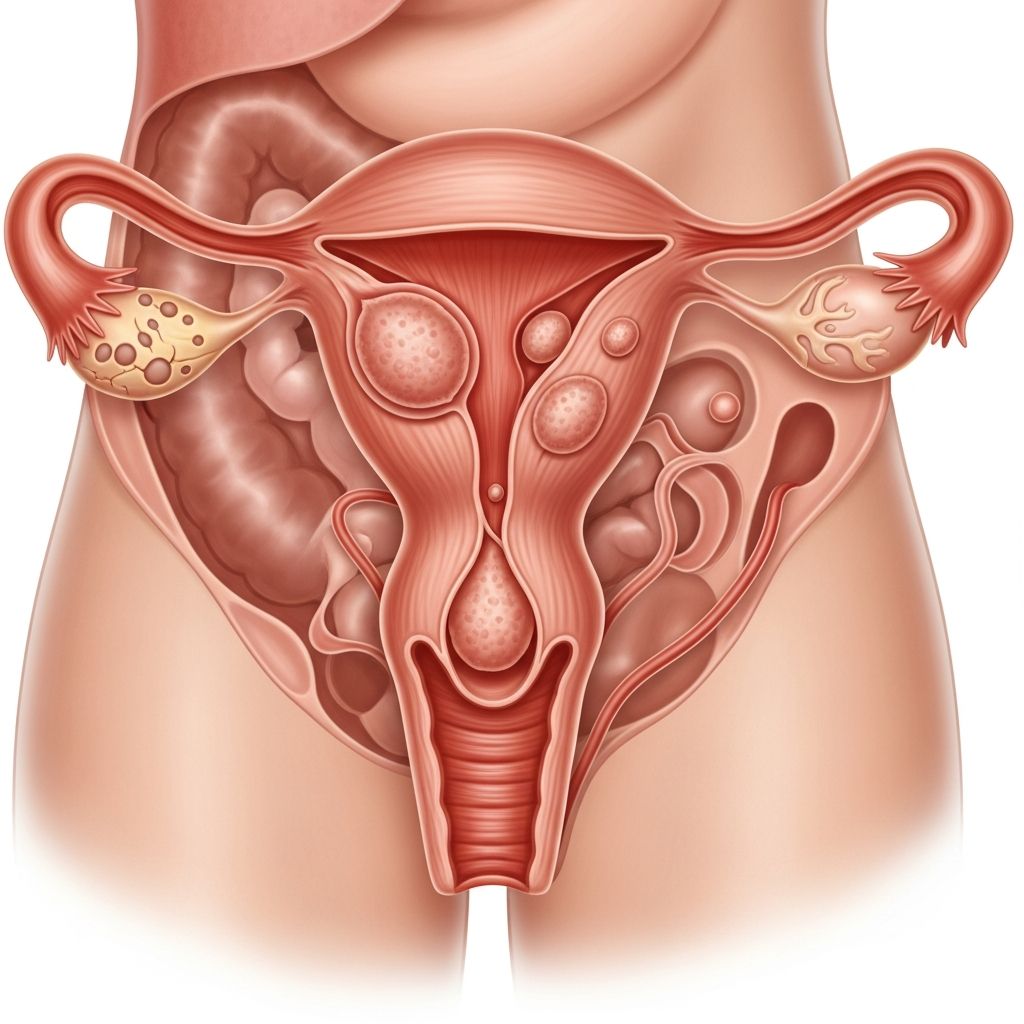
Uterine fibroids are benign (noncancerous) growths that develop in or on the uterus. These growths are extremely common among women of reproductive age, yet many women experience no symptoms and may never require treatment. Understanding what fibroids are, recognizing their symptoms, and knowing the available treatment options can help you make informed decisions about your health and quality of life.
What Are Uterine Fibroids?
Uterine fibroids, also known as leiomyomas or myomas, are smooth muscle tumors that grow within or on the walls of the uterus. Despite their classification as tumors, they are almost always benign, meaning they are not cancerous and do not increase cancer risk. In fact, only 1 in 7,500 women will develop leiomyosarcoma, a rare cancer that can arise from fibroids. These growths vary significantly in size, ranging from microscopic lesions invisible to the naked eye to large masses that can distort the shape of the uterus.
Fibroids can develop in different locations within or around the uterus, which affects how they present and what symptoms they may cause. Some women have a single fibroid, while others may develop multiple fibroids of varying sizes throughout the uterus.
Causes and Risk Factors
The exact cause of uterine fibroids remains unknown, but researchers have identified several factors that may contribute to their development. Hormonal fluctuations, particularly involving estrogen and progesterone, are believed to play a significant role in fibroid growth. These hormones stimulate the uterine lining during each menstrual cycle, and they may also promote fibroid development and proliferation.
Risk factors for developing fibroids include reproductive age, family history, obesity, and certain ethnic backgrounds. Women in their 30s and 40s are more likely to develop fibroids than younger women. Additionally, women with a family history of fibroids face increased risk, suggesting a genetic component to fibroid development.
Symptoms of Uterine Fibroids
Many women with uterine fibroids experience no symptoms whatsoever and discover their condition only incidentally during routine pelvic examinations or imaging studies. However, for those who do experience symptoms, these can significantly impact daily life and quality of living. Common symptoms of uterine fibroids include:
- Heavy menstrual bleeding or prolonged periods
- Pelvic pain and pressure sensations
- Abdominal bloating or enlargement
- Frequent urination or constipation
- Pain during sexual intercourse
- Anemia resulting from heavy bleeding
- Infertility or recurrent miscarriage
The severity of symptoms depends on the size, number, and location of fibroids within the uterus. Submucosal fibroids, which extend into the uterine cavity, are more likely to cause heavy bleeding, while intramural fibroids within the uterine wall may cause pressure symptoms.
When Do Fibroids Require Treatment?
Fibroids only require treatment when they cause problems that interfere with quality of life. Asymptomatic fibroids discovered incidentally do not typically need intervention. However, when fibroids cause heavy bleeding, pain, pressure symptoms such as constipation or frequent urination, or fertility issues, treatment becomes necessary. The decision to pursue treatment is highly individualized and depends on symptom severity, fertility goals, and personal preferences.
Diagnosis and Evaluation
Proper diagnosis of uterine fibroids begins with a detailed medical history and thorough gynecological examination. Your healthcare provider will discuss your symptoms, menstrual patterns, medical history, and medications. Several diagnostic imaging techniques help confirm the diagnosis and determine the location, size, and extent of fibroids.
Diagnostic Methods
Ultrasound: This non-invasive test uses sound waves to create images of your pelvic organs. Ultrasound is often the first test performed to confirm uterine fibroids and check for abnormalities in your pelvis. Both transabdominal and transvaginal ultrasound approaches may be used.
Diagnostic Hysteroscopy: During this procedure, a thin, flexible lighted tube called a hysteroscope is inserted through the vagina to directly examine the inside of the uterus. This allows your healthcare provider to determine the size and extent of fibroids and check for other conditions such as polyps or infections.
Saline Infusion Sonography: This specialized transvaginal ultrasound expands the uterus with salt water while using sound waves to reveal fibroids, polyps, or other abnormal structures within the uterine cavity.
Magnetic Resonance Imaging (MRI): MRI provides detailed images of the uterus and fibroids, offering precise information about fibroid location, size, and number. This imaging is particularly useful when planning surgical interventions.
Non-Surgical Treatment Options
For women who prefer to avoid surgery or have asymptomatic fibroids, several non-surgical approaches can help manage symptoms effectively.
Medical Management
Medical therapy is typically used to treat bleeding associated with uterine fibroids and can help reduce symptoms without surgery. Traditional medical therapies include birth control pills and hormone medications that can be both therapeutic and curative for fibroid-related bleeding. These medications work by regulating menstrual bleeding and reducing heavy flow during periods.
Nonsteroidal anti-inflammatory drugs (NSAIDs) can help manage pain associated with fibroids, while iron supplements may be recommended to prevent or treat anemia resulting from heavy bleeding.
Minimally Invasive Surgical Options
When surgical intervention is necessary, several minimally invasive options are available that preserve the uterus and allow for faster recovery compared to traditional open surgery.
Hysteroscopic Myomectomy
For small fibroids located within the uterine cavity, hysteroscopic myomectomy offers an effective solution. During this procedure, a hysteroscope is inserted through the vagina, and surgical instruments attached to the scope are used to remove fibroids from inside the uterus. This outpatient procedure requires no abdominal incisions, takes minimal time, and allows most women to return to normal activities within a few days.
Laparoscopic and Robotic-Assisted Myomectomy
For larger fibroids or those located in different areas of the uterus, laparoscopic or robotic-assisted myomectomy may be performed. These procedures use small incisions (typically 5-10mm) in the abdomen through which specialized instruments remove fibroids while preserving the uterus. Robotic assistance may be utilized depending on the surgeon’s preference and the complexity of the case. These minimally invasive approaches result in significantly less pain and faster recovery compared to open surgery.
Radiofrequency Ablation (RFA)
Radiofrequency ablation applies heat directly into fibroids, causing them to shrink over time and reducing associated symptoms. This minimally invasive procedure may be performed vaginally or laparoscopically depending on the size, number, and location of the fibroids.
Uterine Artery Embolization (UAE)
In this innovative procedure, interventional radiologists collaborate with gynecologists to place a small catheter into an artery in the groin or wrist. Particles are then injected through the catheter into the uterine arteries to cut off blood supply to the fibroids. This oxygen and nutrient deprivation causes fibroids to shrink over several months. This procedure is particularly suitable for women who do not desire future pregnancy.
Endometrial Ablation
During endometrial ablation, a surgeon uses heat to destroy the lining of the uterus. While this procedure may burn small fibroids near the uterine lining, it is primarily performed to reduce heavy bleeding during periods. Since endometrial ablation affects fertility, it is not recommended for women planning to have children.
MRI-Focused Ultrasonic Ablation
Also called focused ultrasound, this procedure utilizes MRI imaging to accurately localize fibroids while avoiding damage to surrounding tissue. A high-energy ultrasound transducer then heats and destroys fibroid tissue. The fibroids gradually shrink over time following treatment.
Hysterectomy as a Treatment Option
A hysterectomy, surgical removal of the uterus, is the only permanent cure for uterine fibroids. While many women assume they will need an open hysterectomy with a large abdominal incision and extensive recovery, minimally invasive approaches are now possible in most cases.
Minimally Invasive Hysterectomy
Vaginal or laparoscopic hysterectomy requires only small incisions in the abdomen, allowing for significantly faster recovery and less postoperative pain. For women who are premenopausal, ovaries are typically preserved during hysterectomy to avoid early menopause and the need for hormone therapy. Most women can go home the same day as surgery, with a typical recovery period of two to four weeks.
Abdominal Hysterectomy
Open abdominal hysterectomy involves removal of the uterus through a large incision. However, with advances in minimally invasive techniques, an abdominal approach is very rarely indicated for benign conditions like fibroids. If a healthcare provider recommends an open approach for fibroid treatment, seeking a second opinion with a minimally invasive specialist is advisable.
Choosing the Right Treatment
Treatment decisions should be highly personalized and based on multiple factors including symptom severity, fertility goals, fibroid characteristics, overall health, and personal preferences. Healthcare providers should discuss all available options and help patients understand the benefits and limitations of each approach.
At specialized centers, comprehensive evaluation determines whether medical therapy, surgical intervention, or a “wait and see” approach is most appropriate. Careful assessment of menstrual history, health history, medications, and gynecological examination combined with appropriate imaging helps guide treatment recommendations.
Frequently Asked Questions
Q: Are uterine fibroids cancerous?
A: No, uterine fibroids are almost always benign (noncancerous) growths. Only 1 in 7,500 women develop leiomyosarcoma, a rare cancer arising from fibroids. The vast majority of fibroids pose no cancer risk.
Q: Can fibroids affect fertility?
A: Fibroids can potentially impact fertility, particularly if they distort the uterine cavity or affect embryo implantation. However, many women with fibroids conceive without difficulty. Your healthcare provider can assess whether fibroids may be affecting fertility in your specific situation.
Q: What is the recovery time after minimally invasive fibroid removal?
A: Recovery time varies by procedure. Hysteroscopic myomectomy typically requires only one to two days recovery, while laparoscopic procedures usually involve a recovery period of several weeks. Minimally invasive approaches consistently offer faster recovery compared to open surgery.
Q: Will fibroids come back after treatment?
A: After myomectomy (fibroid removal), new fibroids may develop, though the removed fibroids themselves do not regrow. Hysterectomy provides permanent relief since the uterus is removed. Recurrence rates after other procedures vary.
Q: Do all fibroids require treatment?
A: No. Asymptomatic fibroids that cause no problems typically do not require treatment. Treatment is recommended only when fibroids cause symptoms that interfere with quality of life, such as heavy bleeding, pain, or pressure symptoms.
References
- Uterine Fibroids: Causes, Symptoms & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/9130-uterine-fibroids
- Uterine Fibroid Treatment Options — Cleveland Clinic Services. 2024. https://my.clevelandclinic.org/services/uterine-fibroids-treatment
- Center for Menstrual Disorders, Fibroids and Hysteroscopic Services — Cleveland Clinic Department of Obstetrics, Gynecology & Women’s Health. 2024. https://my.clevelandclinic.org/departments/obgyn-womens-health/depts/menstrual-disorders
Read full bio of Sneha Tete











