Varicocele: Causes, Symptoms, Diagnosis & Treatment
Comprehensive guide to understanding varicocele, its causes, symptoms, diagnosis methods, and effective treatment options.
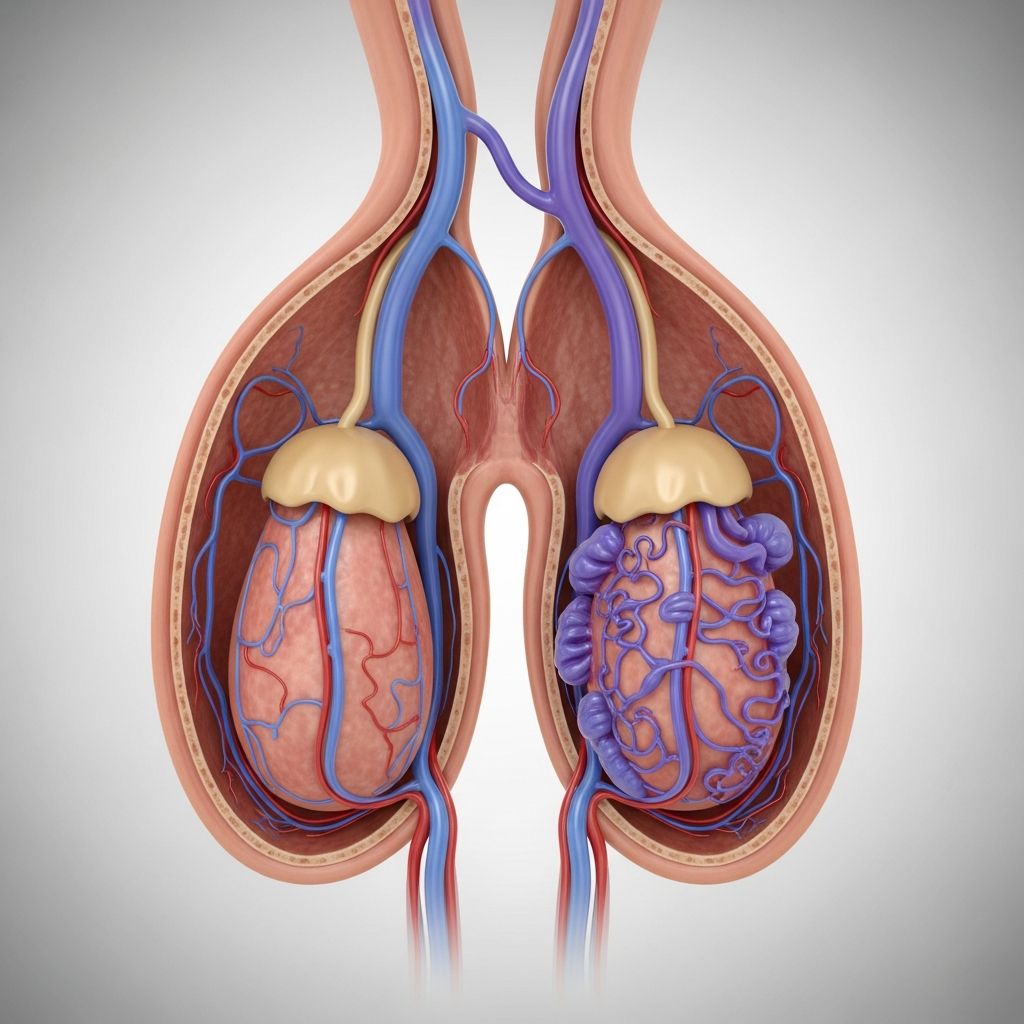
Understanding Varicocele: A Comprehensive Overview
A varicocele is a medical condition characterized by the enlargement of veins within the scrotum, similar to varicose veins that can occur in the legs. This condition affects approximately 15% of men and is one of the most common urological problems encountered in clinical practice. While varicoceles are frequently asymptomatic and discovered incidentally during physical examinations or imaging studies, they can sometimes cause significant discomfort and have been associated with male infertility in some cases. Understanding the nature of varicoceles, their potential causes, symptoms, and available treatment options is essential for men concerned about their reproductive health and overall wellbeing.
What Causes Varicocele?
The exact etiology of varicocele remains not entirely understood by medical professionals, though several well-documented theories explain its development. The most widely accepted theory involves the malfunction of valves within the veins of the spermatic cord. These valves are designed to regulate blood flow and prevent the backflow of blood toward the testicles. When these valves become defective or weak, blood accumulates within the veins, causing them to dilate and enlarge over time.
Another significant contributing factor is the anatomical difference between the left and right testicular veins. The left testicular vein follows a slightly different path than the right vein, inserting into the left renal vein at a right angle. This positioning creates increased pressure and makes blood flow obstruction more likely on the left side, which explains why approximately 85% of varicoceles occur on the left side of the scrotum.
Additional anatomical factors include potential compression of the left renal vein between the abdominal aorta and the superior mesenteric artery, a condition that can increase venous pressure in the left spermatic vein and result in obstruction. Genetic predisposition also plays a role, as varicoceles tend to run in families, suggesting hereditary factors influence their development.
Hormonal changes, particularly during puberty when the testicles undergo rapid growth and require increased blood flow, are believed to contribute to varicocele formation. Environmental factors such as prolonged standing or sitting can increase pressure on the scrotal veins, potentially contributing to their dilation. In rare cases, external factors including tumors, kidney disease, or injuries that disrupt normal blood flow in the scrotal region may cause secondary varicoceles.
Recognizing Symptoms of Varicocele
Many men with varicoceles experience no symptoms whatsoever and discover the condition only during routine physical examinations or when undergoing imaging studies for other reasons. When symptoms do occur, they are typically mild and may include the following:
- Swelling or enlargement of the scrotum, particularly noticeable in the afternoon or after physical activity
- A dull aching pain or discomfort in the affected testicle, which may worsen with prolonged standing or physical exertion
- A feeling of heaviness or fullness in the scrotum
- Visible or palpable enlarged veins within the scrotum, often described as feeling like “a bag of worms”
- Symptoms that typically improve when lying down or wearing supportive underwear
Pain occurs in only 2% to 10% of varicocele patients. The severity of symptoms does not necessarily correlate with the severity of the condition, as some men with large varicoceles experience no discomfort, while others with smaller varicoceles may have significant pain. This variability in symptom presentation underscores the importance of individual assessment and personalized treatment approaches.
Diagnosis and Clinical Evaluation
Healthcare providers typically diagnose varicocele through a combination of clinical examination and imaging studies. During a physical examination, the physician palpates the scrotum to detect enlarged veins, often performing what is known as the Valsalva maneuver, in which the patient bears down to increase intra-abdominal pressure, making varicoceles more apparent.
Scrotal ultrasound is the most commonly used imaging modality for confirming varicocele diagnosis and assessing severity. This non-invasive procedure uses sound waves to visualize the veins within the scrotum and can measure vein diameter and blood flow patterns. Doppler ultrasound may be employed to evaluate venous reflux, providing additional diagnostic information.
In some cases, particularly when secondary varicocele is suspected or when imaging findings are ambiguous, magnetic resonance imaging (MRI) or computed tomography (CT) scans may be ordered to rule out underlying conditions such as renal tumors or other abdominal pathology that could be causing venous obstruction.
Varicoceles are classified into three grades based on clinical and imaging findings. Grade 1 varicoceles are small and palpable only with the Valsalva maneuver. Grade 2 varicoceles are palpable without maneuver but not visible through the skin. Grade 3 varicoceles are large, easily palpable, and visibly apparent through the scrotal skin.
Impact on Fertility and Sperm Production
One of the most significant concerns associated with varicocele is its potential impact on male fertility and sperm production. Several mechanisms have been proposed to explain how varicoceles may affect reproductive capacity. The most widely accepted theory suggests that varicoceles elevate the temperature of the scrotum due to dilated veins and pooling of blood. The increased testicular temperature interferes with normal spermatogenesis (sperm production) and can damage or destroy sperm that has already been created.
Additional proposed mechanisms include increased testicular oxidative stress, higher venous pressure, hormonal imbalances, reflux of toxic metabolites from the kidneys or adrenals, tissue hypoxia, and possible nerve fiber stretching from the dilated varicocele complex.
It is important to note that not all varicoceles cause infertility, and many men with varicoceles father children without difficulty. Men with normal semen analysis do not require treatment for their varicocele. Treatment should be considered when men have associated pain or infertility with an abnormal semen analysis.
Non-Surgical Treatment Options
For mild varicoceles that do not cause significant symptoms or fertility problems, conservative management is often recommended as an initial approach. Non-surgical treatment options include the following:
- Scrotal support through the use of snug-fitting underwear (briefs-style) or a jockstrap, which helps reduce discomfort by providing elevation and reducing venous pooling
- Application of ice packs to the affected area to reduce swelling and provide temporary pain relief
- Over-the-counter pain medications such as ibuprofen, naproxen, or acetaminophen to manage discomfort
- Lifestyle modifications including avoiding prolonged standing, taking frequent breaks during sitting activities, and elevating the scrotum when resting or sleeping
- Limitation of strenuous physical activity that might exacerbate symptoms
These conservative measures are often effective for managing mild symptoms and may be tried for an initial period before considering surgical intervention. However, if symptoms persist or worsen despite these measures, or if infertility remains a concern, surgical treatment should be discussed with a urologist.
Surgical Treatment and Procedures
Surgery, known as varicocelectomy, is the most common treatment for symptomatic varicoceles or those affecting fertility. The procedure involves making a small incision in the groin area to access the spermatic cord containing the enlarged vessels. Once identified, the dilated veins are ligated (tied off) to redirect blood flow into other normal, healthy veins while preserving the testicular artery and other important structures such as the vas deferens.
Surgical Approaches
Several surgical techniques are available for varicocele repair, each with distinct advantages:
- Open retroperitoneal approach: Performed through an incision above the inguinal ligament, providing direct access to the internal spermatic vein at a higher level
- Inguinal approach: Uses an incision in the groin at the level of the inguinal canal
- Subinguinal approach: Performed below the inguinal ligament, allowing for increased magnification and identification of multiple venous branches
- Laparoscopic approach: A minimally invasive technique using small incisions and a camera to visualize the internal spermatic vein
- Microsurgical approach: Utilizes an operating microscope to provide enhanced visualization and precise identification of critical structures, reducing the risk of complications such as testicular artery injury
Microsurgical techniques, increasingly offered at specialized medical centers, have demonstrated superior outcomes in preventing recurrence and minimizing complications by allowing precise identification and preservation of the testicular artery and other vital structures.
Minimally Invasive Alternatives
Percutaneous embolization represents an alternative to traditional surgical repair and is performed in specialized radiological departments. During this procedure, a catheter is inserted into a vein, typically in the groin, and guided to the site of the varicocele using real-time radiological imaging. Once positioned, an embolic agent (such as coils or sclerosing solutions) is deployed to block blood flow through the enlarged veins, causing them to shrink and disappear over time.
Surgical Outcomes and Recovery
Varicocelectomy is typically performed on an outpatient basis under general or local anesthesia, requiring no overnight hospital stay. Pain following surgery is generally mild, and most patients can return to regular activities within two to three days. Complete recovery and return to strenuous activities typically occurs within two to four weeks, depending on the surgical approach used.
Surgical success rates are excellent, with approximately 85-90% of varicoceles successfully treated with no recurrence. Among men undergoing surgery for infertility-related varicoceles, approximately 50% are able to father a child within the first year after treatment, with improvement in semen parameters noted in a higher percentage of patients.
Potential Complications and Risks
While varicocelectomy is generally safe and well-tolerated, potential complications should be discussed with your surgeon prior to the procedure. These may include:
- Recurrence of varicocele (1-15% depending on surgical technique)
- Hydrocele formation (fluid collection around the testicle), occurring in 1-7% of cases
- Testicular artery injury, more common with non-microsurgical techniques
- Bleeding or hematoma formation
- Infection at the surgical site
- Reactions to anesthesia
- Chronic pain or numbness in the surgical area
Discussion of these risks with your surgeon, along with review of their personal complication rates, can help inform your treatment decision.
When Should Varicocele Be Treated?
Treatment decisions for varicocele should be individualized based on several factors:
- Presence of pain or discomfort that significantly impacts quality of life or is not adequately controlled with conservative measures
- Infertility concerns with documented abnormal semen analysis
- Evidence of testicular atrophy (decrease in testicular size or volume)
- Subclinical varicoceles (no pain or fertility concerns) typically do not require treatment
A subclinical varicocele, discovered incidentally without associated symptoms or fertility problems, generally does not require treatment and can be managed with periodic clinical follow-up. However, men with varicoceles who are concerned about fertility should undergo semen analysis to determine whether treatment is warranted.
Frequently Asked Questions
Q: Can varicocele cause permanent damage to the testicles?
A: While varicoceles can affect sperm production, treatment, particularly early intervention, often prevents permanent damage. Once blood flow is restored to normal through surgery or embolization, testicular function can often improve significantly.
Q: Is varicocele hereditary?
A: Yes, genetic factors appear to play a role in varicocele development, as the condition tends to run in families. Having a family history of varicocele may increase your risk.
Q: Can varicocele go away on its own?
A: Varicoceles do not typically resolve spontaneously. However, many varicoceles remain stable and do not progress, particularly if they are asymptomatic and not affecting fertility.
Q: How long does varicocele surgery take?
A: Most varicocele surgeries take between 30 minutes to 1 hour, depending on the surgical approach and complexity of the case.
Q: Can I exercise after varicocele surgery?
A: Light activities can typically be resumed within a few days. Strenuous exercise and heavy lifting should be avoided for 2-4 weeks following surgery, depending on your surgeon’s recommendations.
References
- Varicocele: Causes, Symptoms, Diagnosis & Treatment — UCLA Health, Department of Urology. 2024. https://www.uclahealth.org/medical-services/urology/conditions-treated/male-conditions/varicocele-symptoms-treatment-diagnosis
- Varicocele Diagnosis & Treatment — Aurora Health Care, Urology Services. 2024. https://www.aurorahealthcare.org/services/urology/varicoceles
- Varicoceles: Symptoms, Causes & Treatment — Cincinnati Children’s Hospital Medical Center. 2024. https://www.cincinnatichildrens.org/health/v/varicoceles
- Varicocele Fact Sheet — American College of Obstetricians and Gynecologists (ACOG), Reproductive Facts. 2024. https://www.reproductivefacts.org/news-and-publications/fact-sheets-and-infographics/varicocele-fact-sheet/
- Varicocele — National Center for Biotechnology Information (NCBI), StatPearls. 2024. https://www.ncbi.nlm.nih.gov/books/NBK448113/
- Varicocele: Causes, Symptoms, Diagnosis & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/15239-varicocele
- Varicocele — Symptoms and Causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/varicocele/symptoms-causes/syc-20378771
Read full bio of Sneha Tete











