Vesicoureteral Reflux: Causes, Symptoms & Treatment
Understanding VUR: Learn about causes, symptoms, diagnosis, and effective treatment options for children and adults.
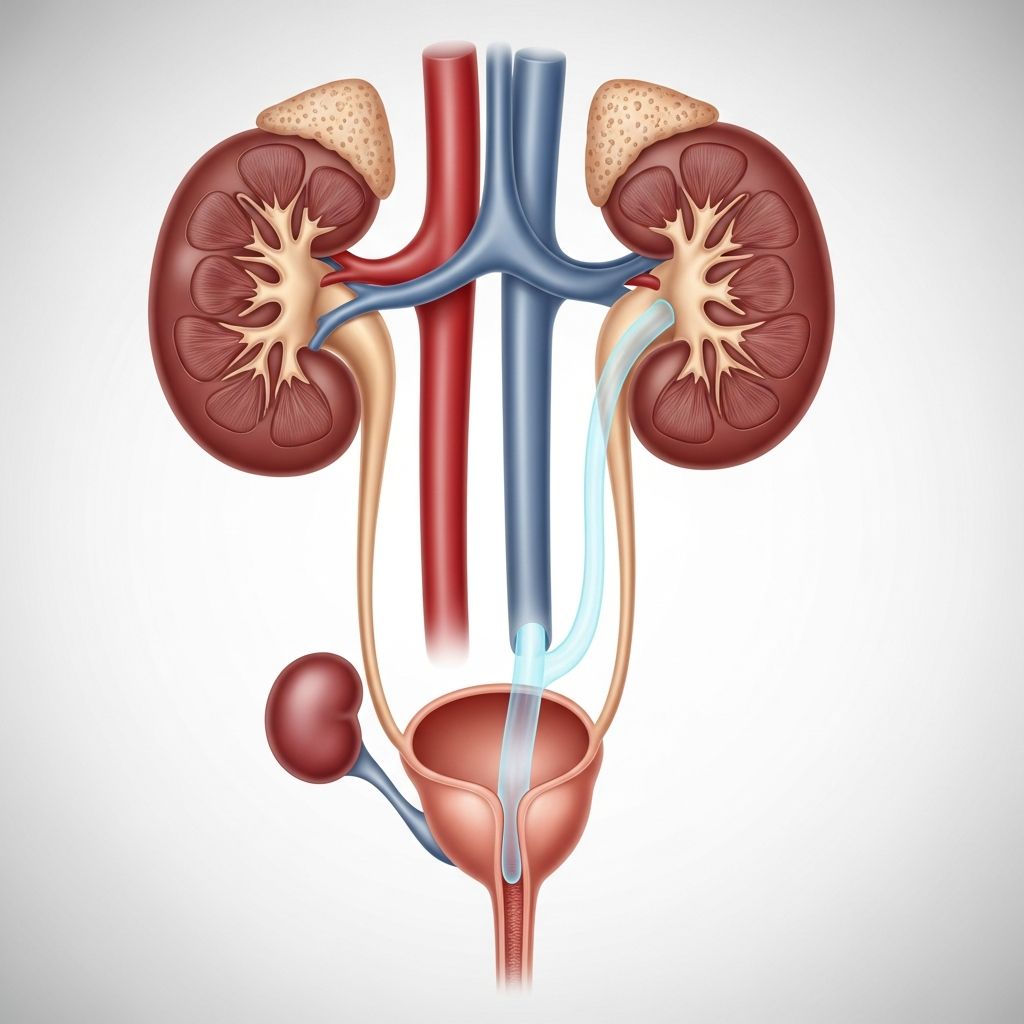
Understanding Vesicoureteral Reflux (VUR)
Vesicoureteral reflux (VUR) is a condition in which urine flows backward from your bladder into one or both of your ureters and, in some cases, up to one or both kidneys. Under normal circumstances, urine travels in one direction only—from your kidneys through the ureters into the bladder and then out through the urethra. However, when VUR occurs, this normal flow is reversed, allowing urine to reflux back toward the kidneys. This happens most often due to an issue that prevents the one-way valve mechanism from functioning properly.
VUR is most common in infants and children, particularly those ages 2 and under, though older children and rarely adults can also develop this condition. The condition itself isn’t usually painful or life-threatening, but it requires proper management to prevent complications such as kidney infections and scarring.
Who Is Affected by VUR?
Vesicoureteral reflux predominantly affects newborns, infants, and young children under the age of 2 years. However, the condition can present in older children and, in rare cases, in adults. When VUR occurs in adults, it is typically associated with other underlying conditions such as benign prostate hyperplasia, neurogenic bladder, or prior surgery near the ureters.
Types of Vesicoureteral Reflux
There are two distinct types of VUR, each with different underlying causes and treatment approaches:
Primary Vesicoureteral Reflux
Primary VUR occurs due to an anatomical abnormality in the valve mechanism between the bladder and ureter. This type is the most common form and is typically present from birth, resulting from a congenital issue with the one-way valve that normally prevents backflow of urine.
Secondary Vesicoureteral Reflux
Secondary VUR develops as a result of another underlying condition or issue, such as a blockage in the urinary tract or dysfunction in how the bladder empties. Unlike primary VUR, secondary reflux is acquired rather than congenital.
Risk Factors for Vesicoureteral Reflux
Several factors can increase the likelihood of developing VUR. Understanding these risk factors can help parents and healthcare providers identify children who may need screening:
- Family history of vesicoureteral reflux
- Recurrent or persistent urinary tract infections
- Abnormalities in kidney or urinary tract structure
- Bladder and bowel dysfunction
- Neurogenic bladder conditions
- Obstructions in the urinary tract
- Male gender (though VUR affects both boys and girls)
Symptoms and Complications of VUR
Common Symptoms
Many children with mild VUR may not experience noticeable symptoms. However, when symptoms do occur, they are often related to associated urinary tract infections. These may include:
- Painful or burning urination
- Frequent urge to urinate
- Urgency and incontinence, particularly in previously toilet-trained children
- Fever without an obvious source
- Abdominal or flank pain
- Cloudy or bloody urine
Associated Bladder and Bowel Dysfunction
Children with VUR may also have bladder and bowel dysfunction (BBD), which includes symptoms such as daytime wetting accidents, nighttime bedwetting, constipation, and incomplete bladder emptying. Children who have VUR along with any BBD symptoms are at greater risk of kidney damage due to infection, making early identification and treatment important.
Potential Complications
The most serious complication of untreated or inadequately managed VUR is kidney damage. VUR itself isn’t life-threatening; however, it can lead to recurrent urinary tract infections (UTIs), which can cause kidney scarring and potentially progress to renal hypertension (high blood pressure from kidney disease) and chronic kidney disease. In severe cases, end-stage kidney disease may require dialysis and/or a kidney transplant. Additionally, VUR can cause kidney stones and stones in other parts of your urinary tract like your bladder.
Most children with VUR recover without long-term complications, particularly when the condition is identified and managed appropriately.
Diagnosis of Vesicoureteral Reflux
Diagnostic Testing
The primary diagnostic tool for identifying VUR is the voiding cystourethrogram (VCUG). This imaging test involves instilling radiopaque contrast medium into the bladder and obtaining images during both filling and voiding phases. A VCUG shows how your urinary tract functions and can reveal whether urine is flowing backward into the ureters or kidneys.
The most common reason to perform a VCUG is to diagnose ureteral reflux in patients with persistent urinary tract infections (UTIs). Your radiologist may assign a score to your test results, especially if your child is the person who had a VCUG.
Grading System for VUR Severity
The severity of vesicoureteral reflux is graded on a scale of 1 to 5, depending on the degree of distention of the collecting system. The rating ranges from one (mild) to five (severe). Grade 1 reflux is the mildest form, where reflux enters only the ureter. Grade 5 represents the most severe form, with massive dilation and tortuosity of the ureter and collecting system. Treatment decisions often depend on how severe the reflux is and whether it’s affecting your kidneys or ureters.
Natural Resolution of Vesicoureteral Reflux
One encouraging aspect of VUR is that reflux resolves spontaneously in many patients. The likelihood of resolution depends on several factors:
- Grade of reflux is the most important factor determining resolution rates
- Lower-grade reflux is more likely to resolve than higher-grade reflux
- Unilateral reflux (affecting one side) is more likely to resolve than bilateral reflux
- VUR not associated with anatomical anomalies resolves more readily
Over several years of observation, reflux resolves in approximately 80 percent of patients with grade 1 or grade 2 reflux, 50 percent of patients with grade 3 reflux and 25 percent of patients with grade 4 reflux. This information helps guide treatment decisions, as many children may outgrow VUR without requiring surgical intervention.
Treatment Options for Vesicoureteral Reflux
Managing VUR requires the help of a healthcare provider. Treatment options depend on your child’s age, symptoms, type of VUR and its severity. Several evidence-based approaches are available:
Antibiotic Therapy
Use of long-term antibiotics for the prevention of UTI is somewhat controversial, as extended use of antibiotics can lead to antibiotic resistance. However, the American Academy of Pediatrics (AAP) recommends preventive antibiotics mostly for children with higher grades of VUR while waiting to see if they outgrow VUR. Low-dose prophylactic antibiotics can help prevent recurrent infections while monitoring the child’s condition.
Deflux Injection (Hyaluronic Acid/Dextranomer)
Deflux® (dextranomer/hyaluronic acid) is a gel-like liquid that offers a minimally invasive treatment option for VUR. Your child’s provider injects a small amount into your child’s bladder wall near the opening of the ureter during cystoscopy. This injection creates a bulge in the tissue and acts like a valve that makes it harder for pee to flow backward. It’s an outpatient procedure (your child goes home the same day), but still requires general anesthesia.
Studies have reported success rates between 70% and 93% for Deflux injections, with higher success rates typically seen in mild to moderate grade VUR. A Deflux implant can treat VUR for up to 25 years, and your own tissue gradually breaks down and replaces the implant over time without losing its effectiveness. Benefits of Deflux compared to other treatments include minimal invasiveness, quick recovery, and effectiveness in preventing urine backflow. However, sometimes VUR and UTIs continue despite treatment, and you may need additional injections if your symptoms continue after one Deflux treatment.
Short-Term Catheterization
In some cases, healthcare providers may recommend short-term catheterization as a temporary measure to allow the urinary system to drain properly while addressing underlying issues or waiting for spontaneous resolution.
Surgical Intervention
Healthcare providers use several different surgical methods for primary VUR. The goal of surgery is to fix the connection point (one-way valve mechanism) between the bladder and ureters to prevent pee from flowing backward.
Ureteral Reimplant is the gold standard procedure for surgical correction of VUR. The goal of the reimplant is to create a flap-valve mechanism, which means re-routing the ureter in the bladder wall with an appropriate length of tunnel so urine doesn’t reflux back up into the ureter. Your child’s surgeon can perform this procedure with an open surgery (incision in your child’s abdomen) or laparoscopically. Surgery requires general anesthesia and possibly a short hospital stay.
Treatment of Secondary VUR
Healthcare providers treat secondary vesicoureteral reflux by removing the blockage or improving how the bladder empties. Treatment may include addressing the underlying cause such as relieving urinary tract obstructions or managing bladder dysfunction.
Managing VUR at Home
Beyond medical interventions, several lifestyle measures can support your child’s overall urinary health:
- Ensure your child drinks plenty of water throughout the day
- Encourage regular physical exercise and activity
- Provide nutritious meals to maintain overall health
- Establish regular bathroom routines
- Maintain proper hygiene practices
- Monitor for signs of urinary tract infections
Living with Vesicoureteral Reflux
If your child receives a VUR diagnosis, working closely with their healthcare team on a treatment plan that works for your family is essential. Managing a condition like VUR can have an effect on you and other caregivers. Be sure to discuss your concerns with your child’s healthcare team.
The good news is that VUR is highly treatable and most children don’t have long-term effects from it. Remember that vesicoureteral reflux isn’t usually painful or life-threatening. It’s manageable and treatments are usually successful. There’s no way to prevent it, but make sure to have your child maintain their overall health through proper hydration, exercise, and nutrition. Rely on your healthcare provider’s expertise—they’ll help diagnose and treat your child’s VUR. Don’t hesitate to contact them with questions and concerns, and be open and honest about your child’s symptoms.
Frequently Asked Questions (FAQs)
Q: Is vesicoureteral reflux life-threatening?
A: VUR itself isn’t life-threatening; however, untreated VUR can lead to recurrent UTIs that cause kidney scarring, potentially leading to kidney disease. With proper management and treatment, most children recover without long-term complications.
Q: Can vesicoureteral reflux be prevented?
A: There is no way to prevent vesicoureteral reflux, as primary VUR is typically a congenital condition. However, maintaining good hydration, proper hygiene, and regular medical monitoring can help prevent associated infections and complications.
Q: Do all children with VUR need surgery?
A: No, not all children with VUR require surgery. Many children, particularly those with lower-grade reflux, may experience spontaneous resolution. Treatment decisions depend on the grade of reflux, presence of infections, and individual patient factors. Your healthcare provider will help determine the best approach for your child.
Q: How long does Deflux treatment last?
A: A Deflux implant can be effective for up to 25 years. The body gradually replaces the injected gel with its own tissue over time, but this doesn’t diminish its effectiveness in preventing urine backflow.
Q: What is the success rate of VUR treatment?
A: Success rates vary depending on the treatment method and grade of reflux. Approximately 80% of patients with grade 1 or 2 reflux experience spontaneous resolution. Deflux injections have success rates between 70-93%, while surgical ureteral reimplant is considered the gold standard with high success rates for correcting reflux.
Q: Can adults develop vesicoureteral reflux?
A: Yes, though it’s rare. Adults typically develop VUR secondary to other conditions such as benign prostate hyperplasia, neurogenic bladder, or prior surgery near the ureters.
References
- Pediatric Urinary Tract Infection and Reflux — American Academy of Family Physicians (AAFP). 1999-03-15. https://www.aafp.org/pubs/afp/issues/1999/0315/p1472.html
- Vesicoureteral Reflux (VUR): Causes, Symptoms & Treatment — Cleveland Clinic. 2024-07-08. https://my.clevelandclinic.org/health/diseases/5995-vesicoureteral-reflux
- Voiding Cystourethrogram (VCUG): Procedure & Results — Cleveland Clinic. https://my.clevelandclinic.org/health/diagnostics/16431-vcug
- Deflux Implant: Treatment for VUR, Procedure & Results — Cleveland Clinic. 2024-07-08. https://my.clevelandclinic.org/health/treatments/16320-deflux-treatment-for-vesicoureteral-reflux
Read full bio of Sneha Tete











