What Causes Osteoarthritis: 4 Common Triggers Explained
Uncover the primary causes and risk factors of osteoarthritis, the most common form of arthritis affecting millions worldwide.
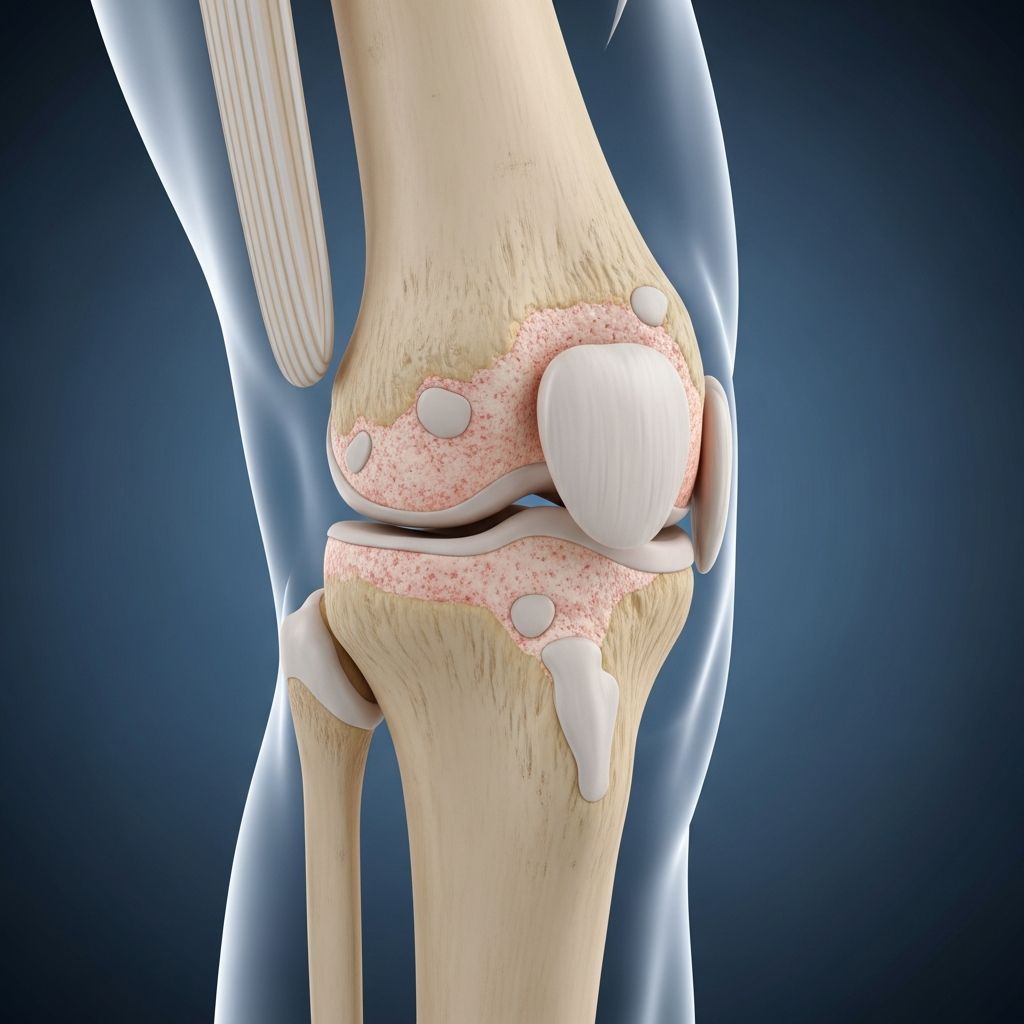
What Causes Osteoarthritis?
Osteoarthritis (OA), the most prevalent form of arthritis, develops when the protective cartilage cushioning bone ends in joints gradually deteriorates, leading to pain, stiffness, and reduced mobility. This degenerative condition primarily impacts joints in the hands, knees, hips, and spine, affecting millions globally and worsening over time without reversing joint damage.
Overview of Osteoarthritis
Osteoarthritis represents a chronic joint disease where the cartilage—a firm, slippery tissue enabling smooth, low-friction movement—wears away progressively. As cartilage thins, bones rub against each other, triggering pain, inflammation, and structural changes in the joint, including bone remodeling and weakening of surrounding ligaments and muscles.
While any joint can be affected, OA most commonly targets weight-bearing areas like knees and hips, as well as the hands and spine. Symptoms emerge slowly, often starting in middle age, and can significantly impair daily activities if unmanaged. Although cartilage loss is irreversible, lifestyle modifications, weight control, and targeted therapies can alleviate symptoms and slow progression.
Symptoms of Osteoarthritis
Osteoarthritis symptoms develop gradually and intensify with time, varying by affected joint. Common manifestations include:
- Pain: Discomfort in the joint during or post-movement, often easing with rest but worsening with overuse.
- Stiffness: Particularly evident upon waking or after inactivity, typically lasting less than 30 minutes.
- Tenderness: Sensitivity when light pressure is applied near the joint.
- Loss of flexibility: Reduced range of motion, making full joint movement challenging.
- Grating sensation: A feeling or audible crepitus (popping/cracking) during joint use.
- Bone spurs: Hard bony growths forming around the joint edges.
- Swelling: Mild inflammation of surrounding soft tissues.
In spinal osteoarthritis, intervertebral disks narrow, and bone spurs develop, potentially compressing nerves and causing radiating pain or numbness. Hip osteoarthritis features cartilage erosion and spur formation, altering gait and leading to groin or thigh pain.
When to See a Doctor
Consult a healthcare professional promptly if joint pain or stiffness persists beyond a few weeks, interferes with daily tasks, or accompanies swelling, redness, or fever. Early intervention can prevent complications and improve quality of life. Those with risk factors like obesity or prior injuries should monitor symptoms closely.
Causes of Osteoarthritis
The fundamental cause of osteoarthritis is the breakdown of articular cartilage, exposing underlying bone and disrupting joint mechanics. This process involves:
- Cartilage degradation: Enzymes and mechanical stress erode the cartilage matrix, reducing its shock-absorbing capacity.
- Bone changes: Subchondral bone thickens and forms osteophytes (spurs) as a response to instability.
- Synovial inflammation: The joint lining may swell, exacerbating damage.
- Ligament and muscle alterations: Weakened support structures impair joint stability.
While aging contributes, OA stems from a multifactorial interplay rather than a single trigger.
Risk Factors for Osteoarthritis
Several modifiable and non-modifiable factors elevate OA risk. Understanding these enables proactive prevention:
| Risk Factor | Description | Impact Level |
|---|---|---|
| Older Age | Risk rises significantly after age 50 as cartilage naturally thins. | High |
| Sex (Female) | Post-menopausal women face higher rates, possibly due to hormonal shifts. | Moderate |
| Obesity | Excess weight stresses weight-bearing joints; adipose tissue releases pro-inflammatory cytokines. | High |
| Joint Injuries | Past trauma (e.g., sports, accidents) disrupts cartilage integrity, even years later. | High |
| Repetitive Stress | Occupations or sports involving joint overuse (e.g., construction, running). | Moderate |
| Genetics | Inherited traits affect cartilage resilience and joint shape. | Moderate |
| Bone Deformities | Congenital issues like dysplastic hips alter joint mechanics. | Moderate |
| Metabolic Diseases | Diabetes or hemochromatosis (iron overload) promotes inflammation. | Low-Moderate |
Obesity exemplifies a dual mechanism: biomechanical load on knees/hips and systemic inflammation from fat-derived proteins.
Complications of Osteoarthritis
Untreated OA progresses, yielding chronic pain that hinders mobility and fosters complications like:
- Functional disability: Difficulty with walking, dressing, or gripping objects.
- Sleep disturbances: Night pain disrupts rest.
- Depression and anxiety: Persistent discomfort impacts mental health.
- Secondary issues: Muscle atrophy, falls, or cardiovascular strain from inactivity.
Advanced cases may necessitate joint replacement surgery.
Prevention and Management Strategies
While OA cannot be fully prevented, risks can be mitigated:
- Maintain a healthy weight to reduce joint stress—losing 5-10% body weight significantly alleviates knee OA symptoms.
- Engage in low-impact exercises like swimming or cycling to strengthen muscles without overload.
- Use protective gear in sports and ergonomics at work to avoid injuries.
- Follow balanced diets rich in anti-inflammatory foods (e.g., omega-3s, antioxidants).
Management includes pain relievers (acetaminophen, NSAIDs), physical therapy, injections, and lifestyle changes. Emerging therapies like gene therapy show promise for knee pain relief.
Frequently Asked Questions (FAQs)
What is the main cause of osteoarthritis?
The primary cause is gradual cartilage wear in joints, leading to bone-on-bone friction, influenced by age and mechanical stress.
Does obesity directly cause OA?
Yes, via increased joint load and inflammatory proteins from fat tissue, especially in hips and knees.
Can OA be reversed?
No, cartilage damage is permanent, but symptoms can be managed effectively to maintain function.
Is OA hereditary?
Genetics play a role, increasing susceptibility through cartilage quality and joint structure traits.
How does injury lead to OA years later?
Injuries alter joint alignment and cartilage health, accelerating degeneration over time.
This comprehensive guide draws from authoritative medical insights to empower better joint health decisions. Early awareness of causes and risks is key to longevity and vitality.
References
- Osteoarthritis – Symptoms & Causes — Mayo Clinic Staff. 2025-04-08. https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925
Read full bio of medha deb











