Causes Of Stomach Cancer: Risk Factors And Prevention
Uncover the key risk factors and causes of stomach cancer, from H. pylori infection to diet and genetics, and learn how to reduce your risk.
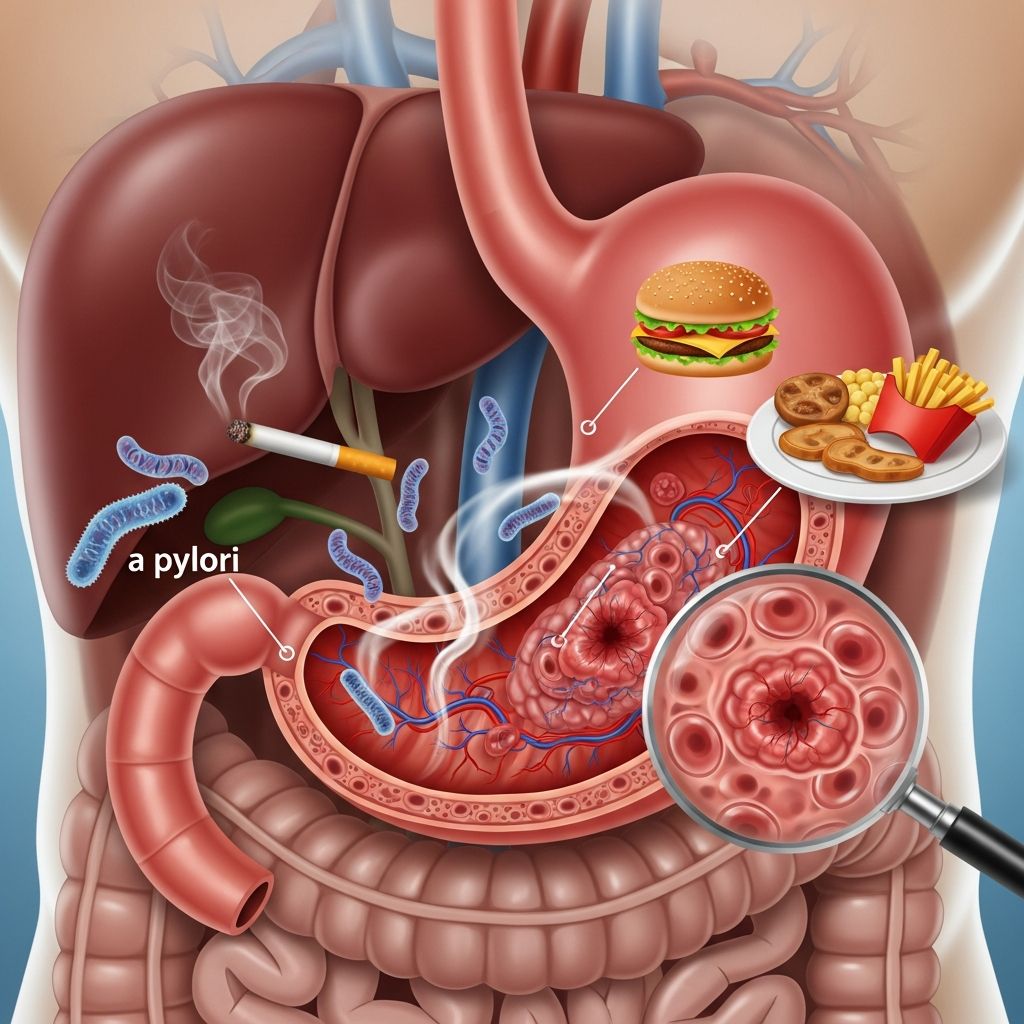
What Causes Stomach Cancer?
Stomach cancer, also called gastric cancer, arises from abnormal changes in the stomach’s lining cells, leading to uncontrolled growth and tumor formation. While the exact cause remains unclear, multiple risk factors like infections, diet, genetics, and lifestyle contribute significantly.
Understanding these factors is crucial for prevention and early detection, as stomach cancer often shows no early symptoms. This article details the primary causes, risk categories, symptoms, diagnosis, treatment, and prevention based on authoritative sources.
What Is Stomach Cancer?
Stomach cancer primarily develops in the inner lining (mucosa) of the stomach and can spread to other layers or organs if untreated. It is more common in people over 60, with higher incidence in certain regions like East Asia, Eastern Europe, and South America.
The most prevalent type is
adenocarcinoma
, originating in mucus-producing cells, accounting for nearly all cases. Other rare types include gastrointestinal stromal tumors (GIST), which start in nerve cells within the stomach wall.Causes of Stomach Cancer
Stomach cancer typically begins with damage to the stomach lining from infections, chronic inflammation, or irritants, causing DNA mutations in cells that lead to overproliferation and tumors. Key triggers include:
- Chronic irritation from acid reflux or H. pylori bacteria altering cell function.
- Long-term inflammation progressing to atrophic gastritis and intestinal metaplasia.
- Genetic mutations accumulated over time, influenced by environmental factors.
Not everyone with these risk factors develops cancer, indicating a complex interplay of genetics and environment.
Risk Factors for Stomach Cancer
Risk factors vary by stomach region: H. pylori affects the lower/middle stomach, while obesity and GERD impact the upper part. They are categorized below.
Infections
Helicobacter pylori (H. pylori) is the strongest risk factor, causing chronic inflammation, ulcers, atrophic gastritis, and cancer. It spreads via saliva, vomit, or stool; treating it reduces risk by up to 30-50% in high-risk groups. Epstein-Barr virus also links to some cases.
Diet and Nutrition
Diets high in salted, smoked, or processed foods (e.g., bacon, sausage, salted fish) increase risk by promoting inflammation and nitrosamine formation. Low fruit/vegetable intake limits protective antioxidants.
| Risky Foods | Protective Foods | Impact |
|---|---|---|
| Salted/smoked meats, pickled vegetables | Fresh fruits, vegetables (high in vitamin C) | Increases risk by 20-50% |
| Red/processed meats | Allium vegetables (garlic, onions) | Moderately elevates risk |
Lifestyle Factors
- Smoking doubles risk by damaging stomach lining and impairing repair.
- Alcohol excess, especially liquor, correlates with higher incidence.
- Obesity raises upper stomach cancer risk via reflux and inflammation.
Medical Conditions
- Chronic atrophic gastritis, pernicious anemia, stomach polyps.
- Gastroesophageal reflux disease (GERD).
Genetics and Family History
Family history or syndromes like hereditary diffuse gastric cancer (HDGC), Lynch syndrome, familial adenomatous polyposis increase risk. Type A blood is a minor factor. Genetic polymorphisms in genes like IL1B, CDH1 also contribute.
Demographic Factors
- Male gender, age over 60, certain ethnicities (Asian, Hispanic, African American).
Signs and Symptoms of Stomach Cancer
Early symptoms mimic indigestion: bloating, heartburn, mild pain. Advanced signs include:
- Unexplained weight loss
- Severe abdominal pain
- Vomiting blood or black stools
- Difficulty swallowing
- Fatigue from anemia
Seek medical advice for persistent symptoms.
Diagnosis and Staging
Diagnosis involves endoscopy, biopsy, CT scans, or PET. Staging (0-IV) determines spread and treatment. Early detection improves 5-year survival from <10% (late-stage) to over 70%.
Treatment Options
Treatment combines surgery (gastrectomy), chemotherapy, radiation, targeted therapy (e.g., HER2 inhibitors), immunotherapy. H. pylori eradication prevents progression in precancerous cases.
Prevention Strategies
- Test and treat H. pylori in high-risk areas.
- Adopt a diet rich in fruits/vegetables, low in salt/processed meats.
- Quit smoking, limit alcohol.
- Manage weight and GERD.
- Genetic screening for high-risk families.
Frequently Asked Questions (FAQs)
Can stomach cancer be prevented entirely?
No, but risk can be reduced by 50-70% through lifestyle changes, H. pylori treatment, and screening.
Is H. pylori infection common?
Yes, over half the global population carries it asymptomatically; eradication is simple with antibiotics.
Does family history mean I’ll get stomach cancer?
It raises risk 2-3x; genetic counseling and screening help manage it.
Are there screening programs for stomach cancer?
Yes, in high-incidence areas like Japan/Korea via endoscopy; not routine elsewhere.
How does diet impact stomach cancer risk?
High-salt/processed food diets increase risk; fruits/veggies decrease it modestly.
This comprehensive overview empowers informed health decisions. Consult healthcare providers for personalized advice.
References
- Stomach Cancer Causes and Risk Factors — National Cancer Institute. 2023. https://www.cancer.gov/types/stomach/causes-risk-factors
- Stomach cancer – Symptoms and causes — Mayo Clinic. 2024-01-16. https://www.mayoclinic.org/diseases-conditions/stomach-cancer/symptoms-causes/syc-20352438
- Risk Factors for Gastric Cancer: A Systematic Review — PMC (National Library of Medicine). 2018-06-07. https://pmc.ncbi.nlm.nih.gov/articles/PMC5980829/
Read full bio of Sneha Tete











