What Happens to Your Body When You Have Insulin Resistance
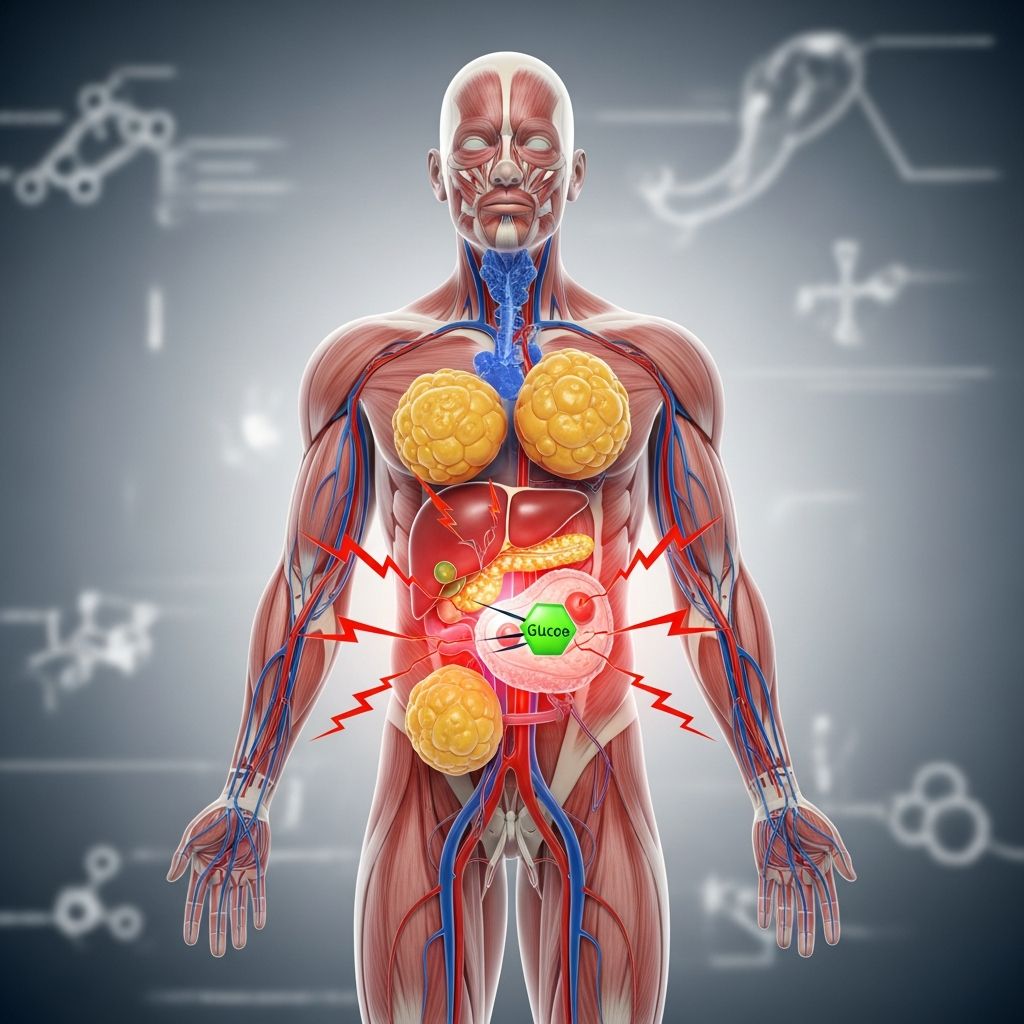
Insulin resistance occurs when your body’s cells—primarily in muscles, fat, and liver—fail to respond effectively to insulin, a hormone that regulates blood sugar by facilitating glucose entry into cells for energy. This leads to elevated blood glucose levels as the pancreas produces more insulin (hyperinsulinemia) to compensate, potentially progressing to prediabetes and type 2 diabetes if unaddressed.
Affecting millions globally, insulin resistance is driven by factors like excess visceral fat, sedentary lifestyles, and poor diet, yet it can be reversed through targeted changes. Understanding its widespread effects across body systems is crucial for prevention.
What Is Insulin Resistance?
Insulin, produced by the pancreas, acts as a key unlocking cells to absorb glucose from the bloodstream, maintaining stable energy levels. In insulin resistance, cells become less responsive, causing glucose buildup (hyperglycemia) and prompting excess insulin release.
Over time, the pancreas may exhaust, failing to produce sufficient insulin, elevating risks for type 2 diabetes and related conditions like cardiovascular disease. Unlike type 1 diabetes (autoimmune), insulin resistance is often lifestyle-acquired, though genetic factors play a role.
Prevalence is high: glucose intolerance, an early IR sign, affected 7.3% of adults (352 million people) in 2017, linked to processed foods, sugars, and inactivity. It manifests in obesity but also underweight individuals with poor habits.
Symptoms of Insulin Resistance
Insulin resistance is often asymptomatic initially, earning its ‘silent’ label, but subtle signs emerge as it worsens. Common symptoms include:
- Fatigue and low energy: Cells can’t utilize glucose efficiently, leaving you tired despite eating.
- Increased hunger and cravings: Hyperinsulinemia disrupts satiety signals, driving sugar cravings.
- Weight gain, especially abdominal: Excess insulin promotes fat storage, particularly visceral fat around organs.
- Skin changes: Dark, velvety patches (acanthosis nigricans) on neck, armpits, or groin signal high insulin.
- Frequent urination and thirst: Emerging hyperglycemia mimics diabetes symptoms.
- Brain fog and irritability: Unstable blood sugar impairs cognitive function.
Many experience no symptoms until prediabetes, underscoring routine screening’s importance via blood tests like fasting glucose or HOMA-IR.
Causes and Risk Factors of Insulin Resistance
Primary causes include lifestyle and physiological factors. Excess body fat, especially abdominal, releases inflammatory adipokines (e.g., TNF-alpha, interleukins) blocking insulin receptors.
Key risk factors:
- Sedentary lifestyle: Lack of activity impairs glucose uptake; obese individuals spend most time sitting.
- Poor diet: High intake of sugars, saturated fats, processed foods, and sweetened drinks; low fruits/vegetables.
- Obesity and visceral fat: Central obesity disrupts metabolism.
- Hormonal imbalances: PCOS, Cushing’s syndrome, or steroids elevate risk.
- Genetics/family history: Rare mutations in insulin receptors or GLUT proteins.
- Age and ethnicity: Risk rises post-45; higher in Hispanic, Black, Native American populations.
- Sleep issues and stress: Chronic cortisol disrupts insulin signaling.
Underweight individuals can develop IR via irregular eating, emotional overeating, or low nutrient intake.
How Insulin Resistance Affects Different Parts of Your Body
Insulin resistance triggers systemic inflammation and metabolic chaos, impacting multiple organs.
Pancreas
Constant overproduction strains beta cells, leading to burnout and insufficient insulin, paving the way for type 2 diabetes.
Liver
Resistant liver cells produce excess glucose (gluconeogenesis) despite high blood levels, worsening hyperglycemia and fatty liver disease.
Muscles
Muscle cells, major glucose users, store less glycogen, causing fatigue and reduced exercise capacity.
Fat Tissue
Impaired signaling promotes fat breakdown, flooding blood with free fatty acids that further block insulin. Visceral fat inflammation exacerbates this.
Brain
Insulin aids brain function; resistance links to cognitive decline, Alzheimer’s risk (‘type 3 diabetes’), and mood disorders.
Heart and Blood Vessels
Hyperinsulinemia raises triglycerides, lowers HDL, promotes plaque, increasing heart disease and hypertension risk.
Kidneys
Chronic high sugar damages filters, risking kidney disease.
Reproductive System
In women, elevates PCOS risk with irregular cycles, infertility; in men, lowers testosterone.
Overall, it fosters metabolic syndrome: abdominal obesity, high blood pressure, dyslipidemia.
Insulin Resistance and Disease Risk
Untreated IR heightens risks for:
- Type 2 diabetes: Primary progression path.
- Cardiovascular disease: 2-3x higher heart attack/stroke risk.
- Nonalcoholic fatty liver disease (NAFLD): Liver fat accumulation.
- PCOS: In 50-80% of cases.
- Certain cancers: Insulin-like growth factor promotes cell proliferation.
- Sleep apnea and osteoarthritis: From obesity.
Diagnosis of Insulin Resistance
No single test; providers use:
- Fasting insulin and glucose for HOMA-IR score.
- A1C (5.7-6.4% prediabetes).
- Oral glucose tolerance test.
- Fasting plasma glucose (100-125 mg/dL impaired).
Physical exam checks waist circumference, skin changes; family history reviewed.
Treatment and Reversal Strategies
Lifestyle is first-line; medications for comorbidities.
Physical Activity
Aerobic (walking, 150 min/week) and resistance training improve sensitivity; even underweight benefit.
Dietary Changes
Focus low-GI foods:
| Foods to Limit | Foods to Emphasize |
|---|---|
| High-GI: Soda, white bread, potatoes, sweets | Low-GI: Oats, legumes, non-starchy veggies, berries |
| Processed meats, fried foods | Fish, poultry, nuts, whole grains |
| Full-fat dairy, trans fats | Low-fat dairy, olive oil, avocados |
Mediterranean, DASH, plant-based diets recommended; 5+ fruits/veggies daily, limit red meat, prioritize steaming/baking. Increase water intake.
Weight Management
5-10% loss dramatically improves sensitivity.
Medications
Metformin, GLP-1 agonists if needed.
Gradual changes yield sustainable results.
Frequently Asked Questions (FAQs)
What is the main cause of insulin resistance?
Excess visceral fat and inactivity are primary; diet high in sugars/processed foods contributes significantly.
Can insulin resistance be reversed?
Yes, often through weight loss, exercise, and diet; early intervention prevents progression.
Does everyone with insulin resistance develop diabetes?
No, manageable cases don’t progress with lifestyle changes.
How is insulin resistance different from prediabetes?
IR precedes prediabetes; prediabetes shows elevated blood sugar on tests.
Can thin people have insulin resistance?
Yes, via poor diet, genetics, or inactivity, as shown in underweight IR patients.
What exercise is best?
Combo of aerobic and resistance; aim 30 min most days.
References
- Eating and Lifestyle Habits in Underweight Patients with Insulin Resistance — PMC/NCBI. 2023-04-28. https://pmc.ncbi.nlm.nih.gov/articles/PMC10122527/
- Insulin Resistance: What It Is, Causes, Symptoms & Treatment — Cleveland Clinic. 2023-07-14. https://my.clevelandclinic.org/health/diseases/22206-insulin-resistance
- What’s the best diet for insulin resistance? — MD Anderson Cancer Center. 2023-01-19. https://www.mdanderson.org/cancerwise/whats-the-best-diet-for-insulin-resistance.h00-159774078.html
- Insulin Resistance and Diabetes — American Diabetes Association. 2024-01-01. https://diabetes.org/about-diabetes/type-2/insulin-resistance
- Pathophysiology of Insulin Resistance — NIH/National Institute of Diabetes and Digestive and Kidney Diseases. 2022-08-15. https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes/prediabetes-insulin-resistance
Read full bio of Sneha Tete