What to Do About Gallstones: Causes, Symptoms, and Treatment
Understanding gallstones: Learn about risk factors, symptoms, diagnosis, and effective treatment options.
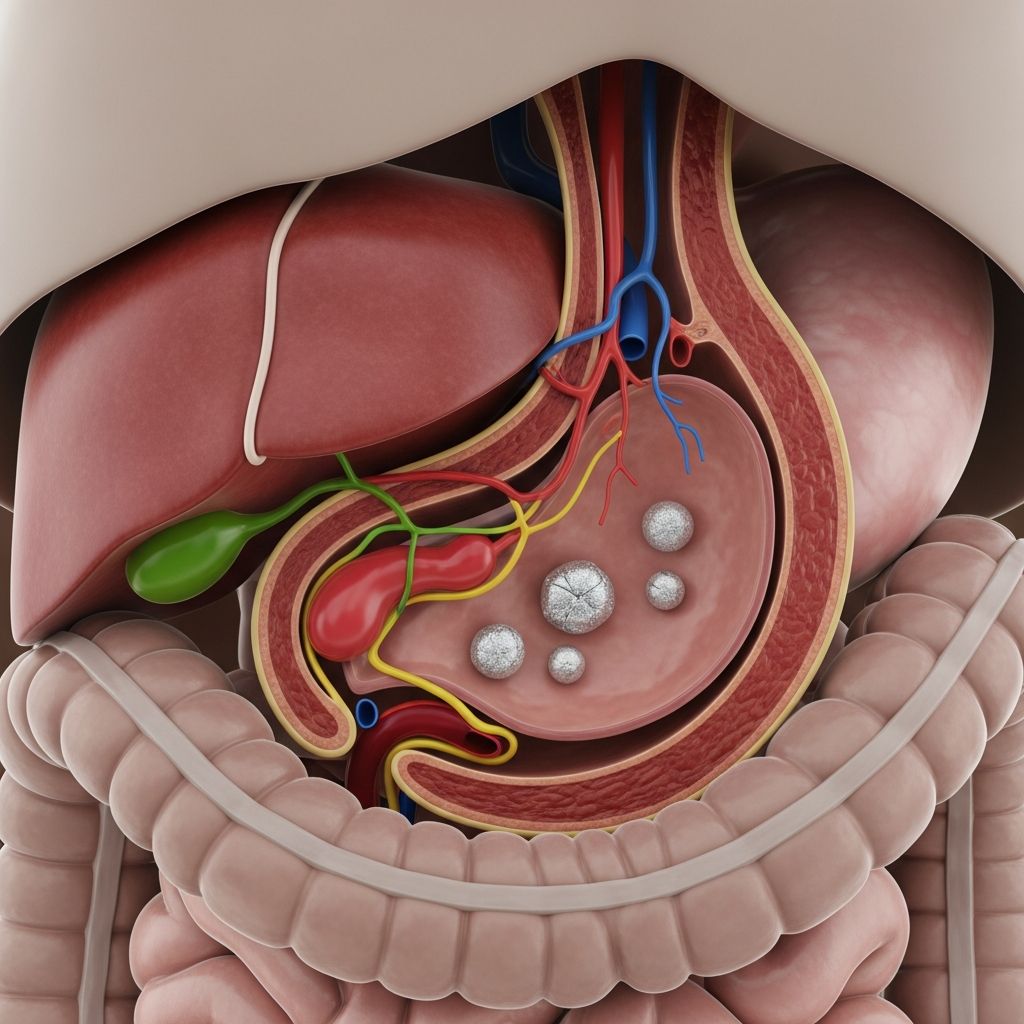
What to Do About Gallstones
Gallstone disease is a common and costly condition affecting millions of people worldwide. It occurs in approximately 10-25% of adults in Westernized countries, resulting in more than 600,000 hospitalizations and 1.8 million ambulatory care visits annually in the United States alone, accounting for over $6.5 billion in annual healthcare costs. Despite a relatively low mortality rate, gallstones can lead to serious complications and significantly impact quality of life. Understanding gallstones, their risk factors, symptoms, and available treatment options empowers individuals to make informed decisions about their health and seek appropriate medical care when necessary.
Understanding Gallstones: What They Are
Gallstones are hardened deposits of digestive fluid that form in the gallbladder, a small organ located beneath the liver on the right side of the abdomen. The gallbladder stores bile, a liquid produced by the liver that helps digest fats. When bile contains excess cholesterol or bilirubin, or when the gallbladder doesn’t empty properly, these substances can crystallize and form stones. These stones can range in size from as small as a grain of sand to as large as a golf ball, and individuals may have one large stone, many small stones, or a combination of both.
Not all gallstones cause problems. In fact, many people have gallstones without experiencing any symptoms, a condition known as silent gallstones. However, when stones obstruct the bile ducts or cause inflammation, they can produce significant discomfort and complications. Understanding the distinction between asymptomatic and symptomatic gallstone disease is crucial for determining appropriate management strategies.
Risk Factors for Gallstone Development
Several factors increase the likelihood of developing gallstones. These risk factors include:
- Age: Gallstones become more common with advancing age, particularly after age 40
- Sex: Women are two to three times more likely to develop gallstones than men, particularly during reproductive years
- Family history: Gallstone disease tends to run in families, suggesting a genetic component
- Obesity: Excess body weight, particularly abdominal obesity, increases cholesterol levels in bile
- Rapid weight loss: Losing weight too quickly can alter bile composition and increase stone formation
- High cholesterol diet: Diets rich in cholesterol and low in fiber promote gallstone development
- Sedentary lifestyle: Physical inactivity increases gallstone risk
- Pregnancy: Hormonal changes during pregnancy can trigger gallstone formation
- Hormone therapy: Estrogen-containing medications increase gallstone risk
- Metabolic syndrome: Conditions like diabetes and insulin resistance are associated with gallstone formation
Research demonstrates that maintaining a healthy lifestyle pattern significantly reduces gallstone risk. Studies have shown that women following a healthy lifestyle score had a 74% lower risk of developing symptomatic gallstone disease compared to those with minimal healthy lifestyle practices, while men following similar patterns experienced an 83% risk reduction. This substantial protective effect underscores the importance of preventive lifestyle modifications.
Recognizing Symptoms of Gallstones
Many people with gallstones experience no symptoms and require no treatment. However, when stones obstruct the bile ducts or cause inflammation, symptoms typically develop. The most common symptom is sudden, severe pain in the upper right portion of the abdomen, a condition called biliary colic. This pain may occur after eating fatty foods and typically lasts from 30 minutes to several hours.
Additional symptoms of symptomatic gallstone disease include:
- Pain between the shoulder blades
- Pain in the right shoulder
- Nausea or vomiting
- Jaundice (yellowing of skin and eyes)
- Dark urine
- Pale-colored stools
- Fever (indicating infection or inflammation)
- Recurring episodes of abdominal discomfort
Symptoms may be triggered by eating fatty, greasy, or heavy meals, though not all gallstone patients experience predictable triggers. Some individuals experience symptoms sporadically, while others may have recurring episodes. It is important to distinguish between gallstone-related pain and other causes of abdominal discomfort, which is why medical evaluation is essential when symptoms arise.
Diagnosis and Medical Evaluation
If gallstone disease is suspected, healthcare providers typically begin with a thorough medical history and physical examination. Several diagnostic imaging tests can confirm the presence of gallstones and assess for complications:
Ultrasound: This is the gold standard imaging test for detecting gallstones. It is noninvasive, widely available, and highly accurate, with a sensitivity exceeding 95% for gallstone detection. Ultrasound uses sound waves to create detailed images of the gallbladder and surrounding structures.
CT Scan: Computed tomography provides detailed cross-sectional images and is particularly useful for identifying complications such as inflammation or infection.
HIDA Scan: This specialized nuclear medicine test evaluates gallbladder function and can detect bile duct obstruction. It involves injecting a radioactive tracer that is taken up by the liver and excreted through the biliary system.
ERCP: Endoscopic retrograde cholangiopancreatography combines endoscopy with X-ray imaging to visualize the bile ducts and is both diagnostic and therapeutic, allowing for stone removal if necessary.
Laboratory Tests: Blood tests measuring liver enzymes, bilirubin, and pancreatic enzymes help identify complications such as bile duct obstruction or pancreatitis.
Treatment Options: Conservative Management
Treatment decisions depend on whether gallstones are symptomatic and whether complications are present. For asymptomatic gallstones, the general recommendation is watchful waiting or conservative management. Most people with silent gallstones never develop symptoms and do not require treatment. Regular follow-up appointments and monitoring for symptom development are typically sufficient.
For symptomatic gallstone disease without complications, several conservative approaches may be considered before surgical intervention:
Dietary Modifications: Following a low-fat diet may help reduce the frequency and severity of symptoms. Avoiding trigger foods such as fried, greasy, and heavy meals can minimize biliary colic episodes. Increasing fiber intake through whole grains, fruits, and vegetables supports digestive health and may promote gallstone dissolution.
Medication: Ursodeoxycholic acid (ursodiol) is a bile acid medication that can dissolve certain types of gallstones over time. However, it works slowly, requires long-term use, and is effective only in select cases with specific stone characteristics. The recurrence rate after discontinuing medication is substantial.
Weight Management: For overweight individuals, gradual weight loss may reduce gallstone symptoms and prevent complications. However, rapid weight loss should be avoided as it can trigger stone formation.
Lifestyle Modifications: Regular physical activity, stress management, and adequate sleep support overall digestive health and may reduce symptom frequency.
Surgical Treatment: Cholecystectomy
When conservative management fails to control symptoms or complications develop, surgical removal of the gallbladder (cholecystectomy) is typically recommended. Cholecystectomy is one of the most commonly performed surgical procedures worldwide, with generally excellent outcomes and high patient satisfaction rates.
Laparoscopic Cholecystectomy: This minimally invasive procedure uses small incisions and specialized instruments to remove the gallbladder. Advantages include shorter recovery time, less postoperative pain, smaller scars, and faster return to normal activities compared to open surgery. Most patients can return home the same day or after an overnight stay.
Open Cholecystectomy: This traditional surgical approach involves a larger incision to directly access and remove the gallbladder. It may be necessary when complications are present or when laparoscopic conversion is needed due to anatomical difficulties.
Robotic-Assisted Cholecystectomy: Some centers offer robotic surgical platforms that provide enhanced visualization and precise instrument control, potentially offering additional benefits in complex cases.
Serious complications from gallstone disease include acute cholecystitis (inflammation of the gallbladder), cholangitis (infection of the bile ducts), gallstone pancreatitis (inflammation of the pancreas), and biliary obstruction. These conditions typically warrant prompt surgical intervention.
Life After Gallstone Treatment
Most patients who undergo cholecystectomy experience complete resolution of symptoms and return to normal activities within weeks to months. The gallbladder stores but does not produce bile, so its removal does not significantly impair digestion. Bile now drips continuously into the intestines rather than being released in measured amounts during meals.
Some patients experience post-cholecystectomy syndrome, characterized by continued abdominal pain or persistent digestive symptoms after surgery. However, this occurs in a minority of patients and may be unrelated to gallbladder removal. Consultation with a gastroenterologist can help identify underlying causes.
Importantly, gallstone recurrence can occur even after cholecystectomy in rare instances when bile duct stones form. Additionally, bile acids have been associated with increased risks of major chronic diseases such as diabetes, cardiovascular disease, and cancer through shared metabolic pathways. Maintaining a healthy lifestyle after treatment helps minimize these long-term health risks.
Prevention Strategies
Adopting a healthy lifestyle pattern significantly reduces gallstone risk. Key preventive measures include:
- Maintaining a healthy body weight through balanced nutrition and regular exercise
- Consuming a high-fiber, low-cholesterol diet rich in fruits, vegetables, and whole grains
- Avoiding rapid weight loss; aim for gradual weight reduction of 1-2 pounds per week
- Engaging in regular physical activity at least 150 minutes weekly
- Limiting saturated fat and refined sugar intake
- Staying hydrated by drinking adequate water
- Managing stress through relaxation techniques and mindfulness
- Discussing medication options with healthcare providers, particularly regarding hormone therapy
Frequently Asked Questions
Q: Can gallstones dissolve on their own?
A: Gallstones rarely dissolve on their own. While medication can dissolve certain types of cholesterol stones in specific situations, most gallstones are permanent. Silent gallstones (those not causing symptoms) do not require treatment and often remain stable indefinitely.
Q: Is surgery necessary if I have gallstones but no symptoms?
A: No, surgery is not routinely recommended for asymptomatic gallstones. Most people with silent gallstones never develop symptoms and do not require surgical intervention. Regular monitoring and observation are typically recommended instead.
Q: What foods should I avoid if I have gallstones?
A: Avoid high-fat foods including fatty meats, fried foods, full-fat dairy products, butter, cream sauces, and processed foods. Trigger foods vary by individual, so keeping a food diary helps identify personal triggers.
Q: How long is recovery after gallbladder removal?
A: Recovery from laparoscopic cholecystectomy typically takes 2-3 weeks for return to light activities and 4-6 weeks for full recovery. Open surgery recovery may require 6-8 weeks or longer.
Q: Will I have digestive problems after gallbladder removal?
A: Most people have no significant digestive problems after gallbladder removal. The body adapts well to continuous bile flow rather than stored bile release. A small percentage experience loose stools or diarrhea, which typically improves with dietary adjustments.
Q: Can gallstones lead to cancer?
A: Gallstone disease has been associated with increased cancer risk through shared risk factors and metabolic pathways, but gallstones themselves do not directly cause cancer. Maintaining a healthy lifestyle reduces cancer risk.
Q: Is gallbladder pain always on the right side?
A: Gallbladder pain is typically in the upper right abdomen, but may also occur between shoulder blades or in the right shoulder. Pain location can vary among individuals.
References
- A healthy lifestyle pattern and the risk of symptomatic gallstone disease in men and women — National Center for Biotechnology Information (NCBI), National Institutes of Health. 2020-09-15. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7458768/
- Gallstone Disease: Clinical Features and Epidemiology — Harvard Medical School, Department of Medicine. 2024. https://www.health.harvard.edu/
- American Gastroenterological Association Medical Position Statement on the Use of Endoscopic Ultrasound — American Gastroenterological Association. 2023. https://www.gastro.org/
- Guidelines on the Management of Common Bile Duct Stones and Acute Cholecystitis — American College of Gastroenterology. 2023-06-01. https://gi.org/
- Epidemiology and Risk Factors for Gallstone Disease in the United States — Centers for Disease Control and Prevention (CDC). 2024. https://www.cdc.gov/
Read full bio of Sneha Tete











