Basal Cell Carcinoma: 5 Stages, Symptoms, And Treatments
Understanding advanced basal cell carcinoma: stages, symptoms, treatments, and prevention strategies for this prevalent skin cancer.
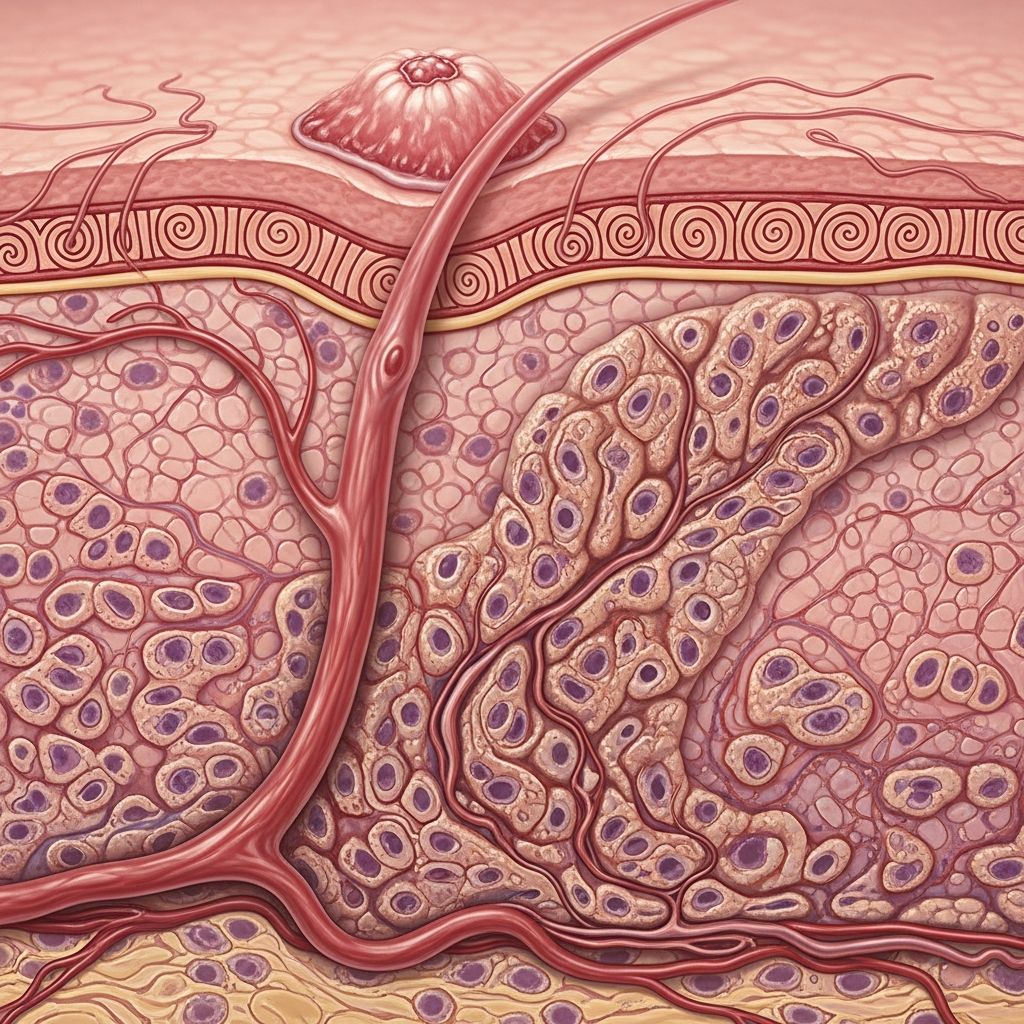
Basal cell carcinoma (BCC) represents over 80% of all skin cancers, originating in the basal cells of the epidermis, primarily on sun-exposed areas like the face and neck. While typically slow-growing and rarely fatal when caught early, advanced BCC can invade deeper tissues or metastasize, necessitating aggressive interventions. This article details its progression, symptoms, staging, treatments, and prevention.
What Is Basal Cell Carcinoma?
BCC arises from uncontrolled multiplication of basal cells in the skin’s outermost layer. It commonly appears on the head, neck, and hands due to cumulative UV exposure. Early BCC is highly curable, but neglect allows deeper invasion or spread.
- **Nodular BCC**: Most common subtype, presenting as a shiny, pearly nodule with telangiectasia (visible blood vessels).
- **Superficial BCC**: Flat, scaly red patch, often mistaken for eczema.
- **Morphoeic/Infiltrative BCC**: Sclerosing, scar-like plaque with ill-defined borders, prone to recurrence.
- **Pigmented BCC**: Blue-black or brown hues, mimicking melanoma.
High-risk factors include fair skin, chronic sun exposure, immunosuppression, and genetic syndromes like basal cell nevus syndrome.
Early Signs of Basal Cell Carcinoma
Initial symptoms are subtle: a persistent pearly bump, non-healing sore, or scaly patch. These lesions grow slowly over months to years, rarely causing pain initially. Regular self-exams and dermatologist visits detect them when treatable via excision or topical therapies.
| Early Appearance | Description | Location |
|---|---|---|
| Pearly nodule | Translucent, rolled edges, central ulceration | Face, ears |
| Scaly patch | Red, itchy, non-healing | Trunk, limbs |
| Open sore | Bleeds easily, crusts over | Sun-exposed areas |
Staging Basal Cell Carcinoma
Staging assesses tumor size, depth, and spread using TNM criteria (Tumor, Node, Metastasis). BCC rarely metastasizes (<0.1%), but local invasion defines advancement.
Stage 0 (Carcinoma in Situ)
Cancer confined to epidermis. Appears as a small (<2cm), flat, scaly, or red patch. No dermal invasion; curable with topical treatments.
Stage 1
Tumor ≤2cm, superficial dermal invasion. Shiny bump or pink patch, no high-risk features. High cure rate with Mohs surgery.
Stage 2
Tumor 2-4cm or <2cm with risk factors (perineural invasion, aggressive histology). May ulcerate or crust; requires wider excision.
Stage 3
Tumor >4cm, invades bone/muscle, or involves nearby nodes. Swollen nodes signal progression; multimodal therapy needed.
Stage 4 (Metastatic BCC)
Rare; spreads to lungs, bones, liver. Symptoms: chronic pain, fatigue, dyspnea, fractures. Systemic therapies essential.
Why Does BCC Advance?
Advancement stems from neglect, immunosuppression, or aggressive subtypes. UV-induced mutations in PTCH1 gene drive growth. Perineural invasion (5-10% cases) heightens recurrence risk. Genetic factors like Gorlin syndrome predispose to multiple BCCs.
- Ignored early lesions grow insidiously.
- Recurrent tumors become infiltrative.
- Immunosuppressed patients (transplant recipients) face 10x risk.
Symptoms of Advanced Basal Cell Carcinoma
Advanced BCC destroys tissue: deep ulcers, bleeding, pain, functional impairment (e.g., eyelid invasion blinds). Metastatic symptoms include weight loss, organ-specific issues like lung metastases causing cough.
- Local effects: Tissue erosion, nerve compression pain.
- Systemic: Fatigue, cachexia in Stage 4.
Diagnosis of Advanced BCC
Biopsy confirms diagnosis. Imaging (MRI/CT) evaluates depth/spread; sentinel node biopsy for nodal involvement. Mohs micrographic surgery aids margin assessment in high-risk cases.
Treatment Options for Advanced BCC
Early stages: Surgery (excision, Mohs), cryotherapy, radiation. Advanced requires:
- Surgery + Radiation: For local control in Stage 3.
- Hedgehog Inhibitors: Vismodegib/sonidegib target SMO pathway; 40-60% response in metastatic BCC.
- Immunotherapy: Cemiplimab for PD-L1 positive advanced cases.
- Clinical Trials: Emerging targeted therapies.
Multidisciplinary care optimizes outcomes; 5-year survival >95% early, drops in metastatic disease.
Prevention and Early Detection
UV protection prevents 90% cases: SPF 30+ sunscreen, UPF clothing, shade. Monthly self-skins, annual dermatology exams crucial. ABCDE rule for moles: Asymmetry, Border irregularity, Color variation, Diameter >6mm, Evolving.
- Avoid tanning beds.
- Check skin head-to-toe monthly.
- Biopsy suspicious lesions promptly.
Frequently Asked Questions
What does advanced basal cell carcinoma look like?
Large, ulcerated, crusted tumors invading deeper tissues; may bleed, cause pain.
Can basal cell carcinoma spread to other organs?
Rarely (Stage 4); lungs, bones common sites.
Is advanced BCC curable?
Yes, often with targeted therapies; early detection best.
How is BCC staged?
TNM system: size, invasion, metastasis.
What increases BCC advancement risk?
Neglect, immunosuppression, sun exposure.
Key Takeaways
- BCC is common but curable early.
- Advanced stages demand specialized care.
- Prevention via sun safety saves lives.
- Regular screenings detect issues timely.
References
- Basal Cell Carcinoma Stages — Cancer Therapy Advisor. 2023. https://www.cancertherapyadvisor.com/factsheets/basal-cell-carcinoma-stages/
- Skin Cancer: Symptoms, Types & Treatment — Cleveland Clinic. 2024-01-15. https://my.clevelandclinic.org/health/diseases/15818-skin-cancer
- Stages and grades of skin cancer — Cancer Research UK. 2024. https://www.cancerresearchuk.org/about-cancer/skin-cancer/stages-grades
Read full bio of medha deb











