Allergic Contact Dermatitis Guide: Causes, Symptoms & Treatment
Understanding the causes, symptoms, diagnosis, and effective treatments for allergic contact dermatitis, a common skin condition triggered by allergens.
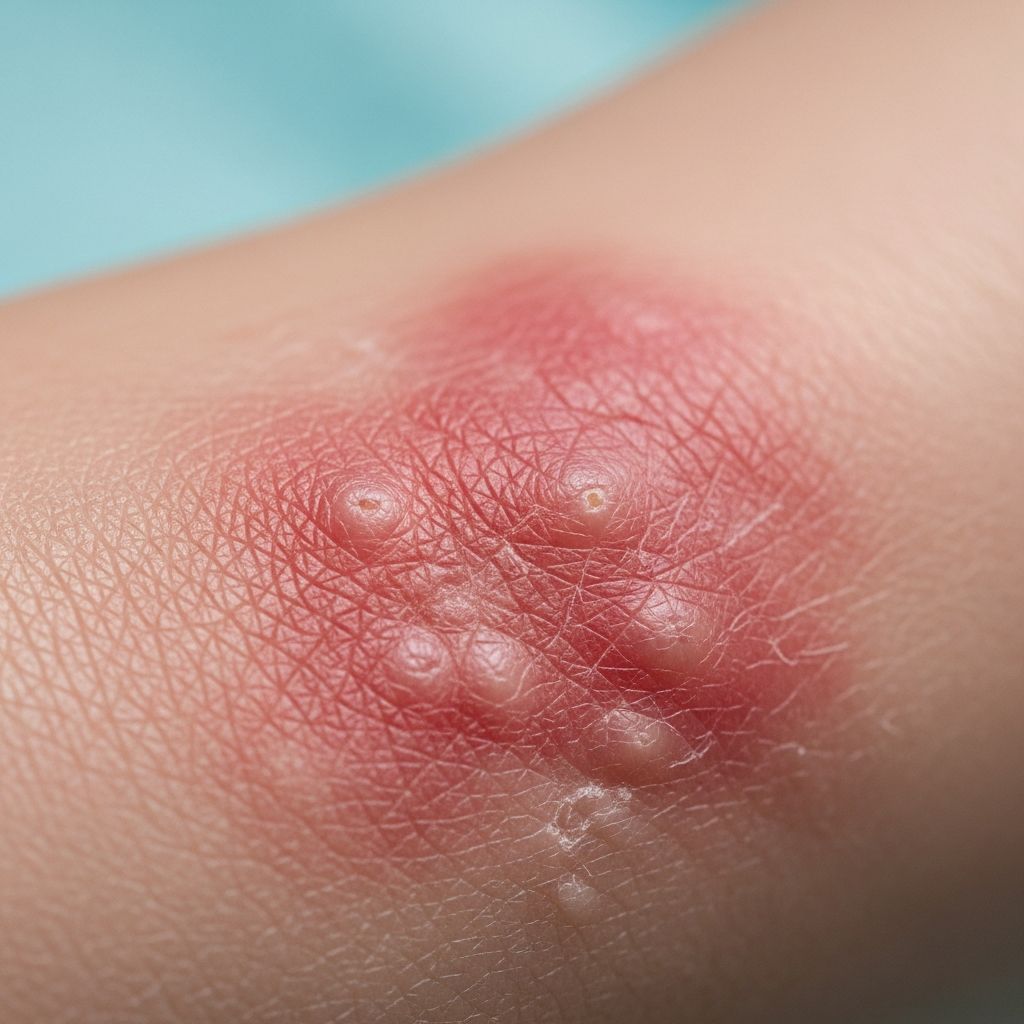
Allergic Contact Dermatitis
Allergic contact dermatitis is a common inflammatory skin condition characterized by an itchy, red rash resulting from a delayed hypersensitivity reaction to specific allergens contacting the skin. It affects people across all ages and occupations, with higher prevalence in those with frequent exposure to potential triggers such as healthcare workers, hairdressers, and construction personnel.
What is allergic contact dermatitis?
Allergic contact dermatitis (ACD) represents a type IV, cell-mediated hypersensitivity reaction mediated by T-lymphocytes, typically manifesting 48–72 hours after initial or repeated exposure to an allergen. Unlike irritant contact dermatitis, which causes direct non-immunologic damage, ACD requires prior sensitization where the allergen binds to skin proteins, forming haptens that activate CD4+ T-cells and trigger cytokine release, leading to inflammation. This delayed onset distinguishes it clinically, with reactions often peaking at 1–3 days post-exposure.
The condition is prevalent, affecting 15–20% of the population at some point, though exact figures vary by region and occupation. It can mimic other eczemas but is distinguished by its geometric patterns corresponding to allergen contact sites, such as linear streaks from plants or ring shapes from jewelry.
Who gets allergic contact dermatitis?
Anyone can develop ACD following sensitization, but risk factors include repeated exposure to allergens in occupational settings (e.g., florists with plant resins, dentists with metals) or daily use of personal care products. Children may react to nickel in earrings or dyes in clothing, while adults often encounter fragrances, preservatives, or rubber accelerators. Genetic predisposition plays a minor role, but environmental exposure is primary. Those with atopic dermatitis have a slightly elevated risk due to impaired skin barrier function.
What causes allergic contact dermatitis?
ACD arises when low-molecular-weight chemicals (haptens) penetrate the stratum corneum, conjugate with proteins, and elicit T-cell responses upon re-exposure. Common allergens include:
- Metals: Nickel sulfate (earrings, buttons), cobalt, chromate (cement).
- Fragrances and plants: Balsam of Peru, urushiol in poison ivy/oak.
- Preservatives: Formaldehyde releasers, parabens in cosmetics.
- Rubber additives: Thiurams, mercaptobenzothiazole in gloves.
- Topical medications: Neomycin, bacitracin in ointments.
Over 4,000 substances can cause ACD, with photoallergic variants triggered by UV-exposed chemicals like sunscreens.
What are the clinical features of allergic contact dermatitis?
Symptoms emerge 24–72 hours post-exposure: acute phase shows erythematous papules, vesicles, bullae, and intense pruritus; chronic exposure leads to lichenification, scaling, and fissuring. Distribution is key—periorbital from nail varnish, hands from gloves, anogenital from wipes. Severe cases may involve id reactions (autoeczematization) or lymphomatoid features mimicking lymphoma.
| Acute Features | Chronic Features |
|---|---|
| Erythema, vesicles, oozing, crusting | Thickening, scaling, hyperkeratosis |
| Intense itch, burning | Mild itch, pain from fissures |
| Well-demarcated, geometric patterns | Diffuse lichen simplex |
Infections can complicate with secondary bacterial involvement, causing pustules or fever.
Diagnosis of allergic contact dermatitis
Diagnosis combines history, exam, and patch testing—the gold standard for confirming allergens. Patch tests apply standardized allergens (e.g., TRUE Test panels) under occlusive patches for 48 hours, read at days 2 and 4–5 for reactions graded as + to +++. True positives show relevance to exposure history; false positives/negatives occur but are minimized with experienced interpretation. Differential includes irritant dermatitis, atopic eczema, tinea, or psoriasis; biopsy rarely helps as histology is non-specific.
How is allergic contact dermatitis treated?
Primary treatment is allergen avoidance after identification. Symptomatic relief includes:
- Topical corticosteroids: Mid-to-high potency (e.g., clobetasol 0.05%, triamcinolone 0.1%) for localized acute lesions; low-potency (desonide) for face/eyelids.
- Systemic steroids: Prednisone taper for >20% body surface involvement.
- Adjuncts: Emollients, cool compresses, oral antihistamines; calcineurin inhibitors (tacrolimus) for steroid-sensitive areas.
Avoid rupturing vesicles to prevent infection; barrier creams aid prevention.
Complications of allergic contact dermatitis
Untreated, chronicity leads to post-inflammatory hyperpigmentation, scarring, or secondary infections. Occupational impairment, anxiety from chronic itch, or erythroderma in widespread cases. Persistent exposure risks occupational disability.
Prevention of allergic contact dermatitis
Prevention hinges on avoidance: substitute allergens, use protective gloves (nitrile over latex), hypoallergenic products. Legislative bans (e.g., certain dyes) and education reduce incidence. Patch testing enables personalized prevention.
Establishing a presumed diagnosis of allergic contact dermatitis
Suspect ACD in eczemas with exposure history, geometric patterns, or refractory to standard therapy. Urgent patch testing if occupational impact suspected.
Management of confirmed allergic contact dermatitis
Tailor to severity: educate on allergen avoidance lists (e.g., from databases like IVDK), provide Information Sheets, refer to dermatology for complex cases. Monitor for cross-reactors (e.g., nickel-cobalt).
Patch testing for allergic contact dermatitis
Performed by specialists using 30–80 allergens; extended series for occupationals. Positive if relevant; patients receive allergen info for shopping/label reading.
Patient outcomes for allergic contact dermatitis
Outcomes excel with avoidance—90% resolve; persistence in 20–50% due to unrecognized exposures. Quality of life improves post-diagnosis.
Frequently Asked Questions
What does allergic contact dermatitis look like?
Typically red, itchy patches with vesicles acutely; thickened skin chronically, patterned to contact.
Can allergic contact dermatitis be cured?
Not cured but managed indefinitely via avoidance; flares cease with compliance.
How long does allergic contact dermatitis last?
Acute episodes 2–4 weeks with treatment; chronic indefinite without avoidance.
Is allergic contact dermatitis contagious?
No, it’s immunologic, not infectious.
Does allergic contact dermatitis go away on its own?
Yes if allergen removed early; otherwise worsens.
References
- Allergic Contact Dermatitis Symptoms and Treatment — St. John’s Physician Partners. 2023. https://www.sjpp.org/dermatology/conditions/rashes/allergic-contact-dermatitis/
- Diagnosis and Management of Contact Dermatitis — American Academy of Family Physicians. 2010-08-01. https://www.aafp.org/pubs/afp/issues/2010/0801/p249.html
- Allergic Contact Dermatitis — StatPearls, NCBI Bookshelf, National Center for Biotechnology Information. 2023. https://www.ncbi.nlm.nih.gov/books/NBK532866/
- Contact Dermatitis – Treatment — National Health Service (NHS). 2023. https://www.nhs.uk/conditions/contact-dermatitis/treatment/
- Contact Dermatitis – Symptoms and Causes — Mayo Clinic. 2023. https://www.mayoclinic.org/diseases-conditions/contact-dermatitis/symptoms-causes/syc-20352742
Read full bio of medha deb











