Cold Urticaria: Quick Guide To Symptoms, Diagnosis & Treatment
Understanding cold urticaria: symptoms, causes, diagnosis, and effective management strategies for this rare hives condition.
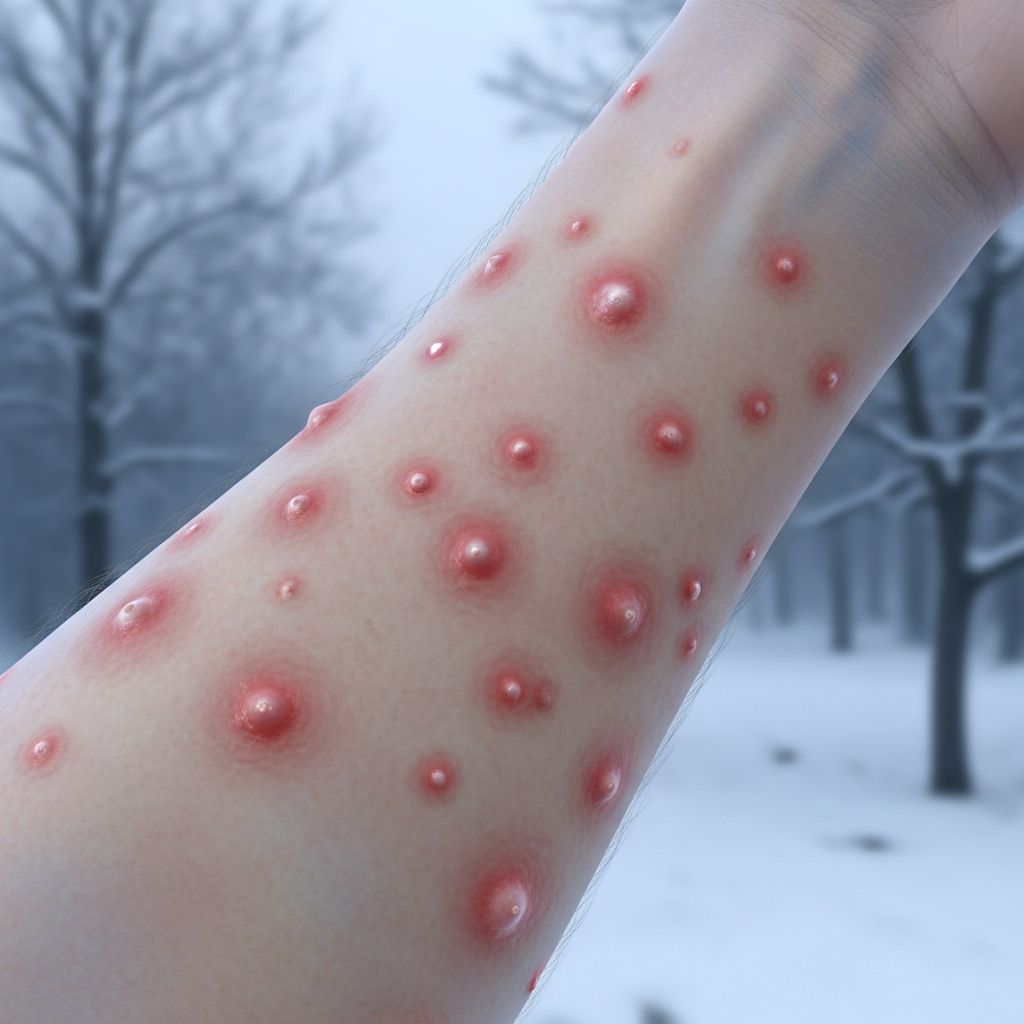
Cold urticaria
Authoritative facts about cold urticaria (cold hives): What it is, who gets it, symptoms, causes, how it’s diagnosed, what it looks like, treatment, prevention, and outlook.
What is cold urticaria?
Cold urticaria is a relatively uncommon form of chronic inducible urticaria in which urticarial weals (hives) develop after being exposed to cold air, cold water, and/or cold objects (eg, ice-cream, ice cubes or cold packs). It is also called cold hives or cold allergy, although it is not a true allergy but rather a sensitivity mediated by mast cell activation.
The hives are usually only confined to the exposed areas but can become more widespread if larger areas of the body are exposed to cold or if the body is rewarmed too quickly. In severe cases, cold urticaria can lead to systemic reactions including anaphylaxis, particularly after immersion in cold water.
Who gets cold urticaria?
Cold urticaria most commonly affects young adults, particularly women, but it can occur at any age. Familial cold urticaria is rare and inherited in an autosomal dominant manner.
Primary acquired cold urticaria is the most common form and affects people aged 20–30 years. Secondary cold urticaria occurs in association with underlying diseases such as hepatitis B or C, monoclonal gammopathy or cryoglobulinaemia.
What causes cold urticaria?
The trigger for cold urticaria is exposure to cold (air, water, objects) followed by rewarming of the skin, which causes activation of skin mast cells. Mast cell degranulation releases histamine and other inflammatory mediators (prostaglandins, leukotrienes), leading to the characteristic hives.
In primary acquired cold urticaria, the cause is unknown (idiopathic). In secondary cold urticaria, there is an identifiable underlying condition.
Familial cold urticaria (also known as familial cold autoinflammatory syndrome) is caused by mutations in the NLRP3 gene, leading to overproduction of interleukin-1β.
Types of cold urticaria
- Primary acquired cold urticaria: Most common; unknown cause; lasts 4–10 years.
- Secondary cold urticaria: Associated with infections (eg, Hepatitis B or C, syphilis), haematological disorders (eg, cryoglobulinaemia, myeloma), autoimmune disease.
- Familial cold urticaria: Autosomal dominant; onset in infancy; burning rather than itchy weals.
Signs and symptoms of cold urticaria
Symptoms of cold urticaria occur within minutes of cold exposure and resolve within 1–2 hours after rewarming.
- Itchy or burning red weals or hives on cold-exposed skin; weals are typically 1–2 cm but can coalesce.
- Swelling (angio-oedema) of hands, lips, tongue, throat, and conjunctivae after holding cold objects or wind exposure.
- Systemic symptoms: Headache, dizziness, weakness, fast heart rate (tachycardia), low blood pressure (hypotension), fainting (syncope), anaphylaxis.
Symptoms are more severe after exposure to cold water (eg, swimming).
Complications of cold urticaria
- Anaphylaxis: Can be fatal; risk increased after swimming in cold water.
- Hydrostatic urticaria: Exacerbation of symptoms due to increased blood flow to dependent areas when immersed in water.
Diagnosis of cold urticaria
The diagnosis of cold urticaria is based on the history and confirmed by a cold provocation test.
Cold provocation test
Ice cube test: An ice cube wrapped in a plastic bag or moistened cloth is placed on the volar forearm for 5 minutes. A weal develops within 10 minutes of rewarming and lasts up to 1 hour.
- Positive test: Weal ≥ 1.5 cm in diameter.
- Sensitivity can be increased by testing other sites or using a TempTest device.
Tests for secondary cold urticaria
- Full blood count, erythrocyte sedimentation rate (ESR).
- Liver function tests, hepatitis serology, serum protein electrophoresis, cryoglobulins, cold agglutinins, antinuclear antibody.
Threshold testing
Temperature threshold: lowest temperature causing a weal (usually 0–15°C).
Duration threshold: longest cold exposure without a weal.
What does cold urticaria look like?
Images shown below are of cold urticaria after ice cube test.
- Red itchy weals on the forearm after ice cube test.
- Swollen hands after holding cold object.
- Lip swelling after cold wind exposure or ice lolly.
Treatment of cold urticaria
The aim of treatment is to reduce the severity of cold-provoked weal and flare reactions.
Education
- Avoid cold triggers when possible.
- Wear warm protective clothing.
- Prewarm intravenous fluids and injection solutions.
- Avoid swimming in cold water (high risk of anaphylaxis).
- Carry an adrenaline autoinjector if history of systemic reactions.
Medications
| Drug | Dose | Notes |
|---|---|---|
| Second-generation H1 antihistamines | Standard or up to 4x dose | First-line; eg, cetirizine, loratadine, fexofenadine. |
| Omalizumab | 300 mg/4 weeks | For antihistamine-refractory cases. |
| Ciclosporin | 3–5 mg/kg/day | For severe refractory cases. |
Investigational treatments
- Cold desensitisation: Daily cold exposure starting at highest tolerated temperature and decreasing by 1°C every 2 days.
Prevention of cold urticaria
- Avoid triggers: cold air, water, objects.
- Protective clothing: gloves, hat, scarf in cold weather.
- Pre-treat with antihistamines before cold exposure.
- Warm up slowly after cold exposure.
Outlook for cold urticaria
Primary acquired cold urticaria remits spontaneously in 50% within 5 years and 85% by 10 years. Familial cold urticaria is lifelong.
Frequently asked questions about cold urticaria
Is cold urticaria dangerous?
Yes, it can cause anaphylaxis, especially after swimming in cold water. Always carry adrenaline if you have had systemic symptoms.
Can cold urticaria be cured?
No cure, but symptoms often improve with time and treatment. Primary form resolves in most within 10 years.
How is cold urticaria diagnosed?
By history and positive ice cube test (weal after 5 min ice on skin).
What should I avoid with cold urticaria?
Cold drinks, ice cream, swimming in cold water, cold showers, air conditioning on bare skin.
Is omalizumab effective for cold urticaria?
Yes, highly effective in antihistamine-resistant cases (300 mg monthly).
References
- Cold Urticaria — NORD (National Organization for Rare Disorders). 2023. https://rarediseases.org/rare-diseases/urticaria-cold/
- Cold-induced urticaria: challenges in diagnosis and management — PMC (PubMed Central). 2013-07-26. https://pmc.ncbi.nlm.nih.gov/articles/PMC3736478/
- Cold Urticaria: What It Is, Symptoms, Causes & Treatment — Cleveland Clinic. 2023-10-04. https://my.clevelandclinic.org/health/diseases/24629-cold-urticaria
- Cold urticaria – Symptoms & causes — Mayo Clinic. 2023-08-03. https://www.mayoclinic.org/diseases-conditions/cold-urticaria/symptoms-causes/syc-20371046
- Understanding cold induced urticaria — Anaphylaxis UK. 2023. https://www.anaphylaxis.org.uk/understanding-cold-induced-urticaria/
- Cold urticaria — UM Health-Sparrow. 2023. https://www.uofmhealthsparrow.org/departments-conditions/conditions/cold-urticaria
Read full bio of Sneha Tete











