Contact Dermatitis: Causes, Symptoms, and Treatment
Learn about contact dermatitis: types, triggers, symptoms, diagnosis, and effective treatment options.
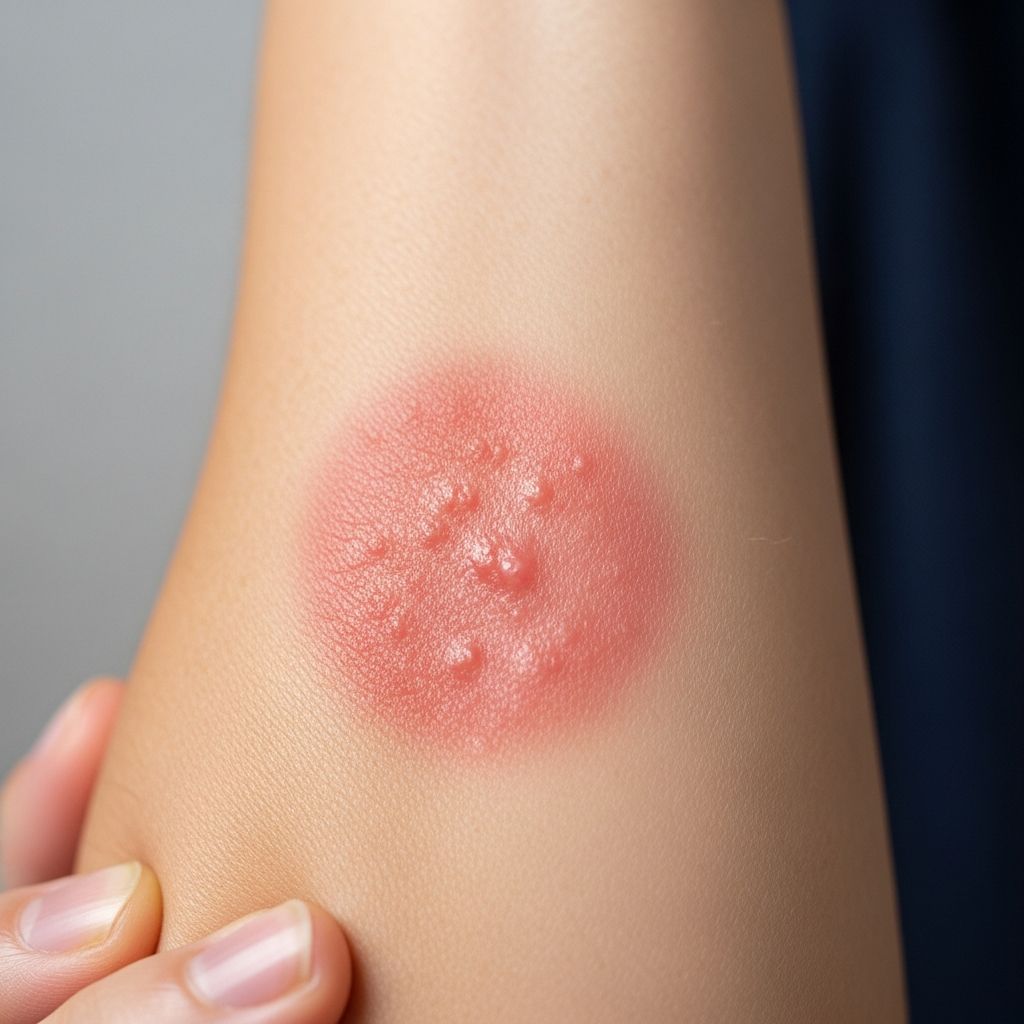
Contact Dermatitis: A Comprehensive Guide
Contact dermatitis is a common inflammatory skin condition that develops when your skin comes into direct contact with a substance that either irritates the skin barrier or triggers an allergic reaction. The condition presents as an itchy, red rash that can range from mild to severe depending on the type of exposure and individual sensitivity. Unlike some skin conditions, contact dermatitis is not contagious, though it can be uncomfortable and may significantly impact daily activities.
Understanding the Two Types of Contact Dermatitis
Contact dermatitis is classified into two distinct categories based on the underlying mechanism of skin irritation:
Irritant Contact Dermatitis
Irritant contact dermatitis occurs when the skin comes into direct contact with a substance that damages the outer layer of the skin through direct chemical damage. Unlike allergic reactions, irritant contact dermatitis does not involve the immune system’s sensitization process. Instead, it results from the substance causing direct cellular damage that releases inflammatory mediators from epidermal cells.
The development of irritant contact dermatitis depends on the duration, intensity, and concentration of the offending substance. Repeated or prolonged exposure significantly increases the likelihood of developing this type of dermatitis. Physical factors such as friction, abrasions, and occlusion combined with chemical irritants can produce more severe reactions than either factor alone. Common irritants include:
- Water from frequent handwashing
- Soaps, detergents, and cleaning products containing sodium lauryl sulfate
- Bleach and other industrial chemicals
- Acidic substances such as lemon juice
- Nail polish remover
- Body fluids and resins
- Hair dyes
The rash from irritant contact dermatitis typically appears within minutes of exposure, making it easier to identify the causative agent.
Allergic Contact Dermatitis
Allergic contact dermatitis develops when the immune system reacts to a specific substance it has become sensitized to. This condition is classified as a delayed-type (Type IV) hypersensitivity reaction, meaning the immune response involves T-cell mediated inflammation. Unlike irritant contact dermatitis, allergic contact dermatitis requires prior exposure to develop sensitization before a visible reaction occurs.
Allergic contact dermatitis occurs in two phases. During the sensitization phase, the body’s dendritic cells capture the allergen and migrate to lymph nodes, where antigen-specific T cells are generated. In the elicitation phase, subsequent exposure activates these T cells in the skin, producing chemical mediators that cause inflammation and the characteristic rash. This process typically takes hours or even days to manifest after exposure, which can make identifying the allergen more challenging than with irritant contact dermatitis.
Common allergens that trigger allergic contact dermatitis include:
- Plants such as poison ivy, poison oak, and poison sumac
- Certain metals including nickel and chromium
- Skincare and beauty products containing fragrances and preservatives
- Rubber and latex
- Medications and topical agents
- Chemical preservatives in cosmetics
Recognizing Symptoms of Contact Dermatitis
The symptoms of contact dermatitis can vary significantly depending on the type, severity, and duration of exposure. Common presentations include:
- Itching: Often the primary symptom, ranging from mild to severe
- Redness: Affected areas display visible erythema or redness
- Dry skin: The affected area becomes dry and uncomfortable
- Rash: Red papules and plaques develop on the contact site
- Blistering: In severe cases, fluid-filled blisters or weeping rash may develop
- Scaling: With prolonged contact, the skin becomes thick and scaly
- Swelling: Inflammation causes visible swelling of affected tissues
The severity of symptoms depends on several factors including the concentration of the irritant or allergen, the duration of contact, the individual’s sensitivity level, and the location on the body. Areas with thinner skin or higher moisture content may be more susceptible to severe reactions.
Causes and Risk Factors
Contact dermatitis develops when sensitized or irritated skin encounters triggering substances. Occupational exposure represents a significant risk factor, as workers in healthcare, construction, cleaning services, and manufacturing frequently encounter irritants and allergens. Certain individuals demonstrate increased susceptibility based on:
- Personal or family history of atopic dermatitis or eczema
- Genetic predisposition to allergic reactions
- Frequency and duration of exposure to irritants
- Compromised skin barrier from existing dermatological conditions
- Age and skin sensitivity variations
- Environmental humidity and temperature conditions
Additionally, photo contact dermatitis represents a unique variant where an allergen becomes an irritant only in the presence of ultraviolet light, causing lesions confined to sun-exposed areas despite broader contact.
Diagnosis of Contact Dermatitis
Accurate diagnosis of contact dermatitis begins with a thorough clinical history and physical examination. Healthcare providers assess the location, appearance, and distribution of the rash to determine the likely type and cause. A careful history of recent exposures, occupational activities, and product use helps identify potential triggering substances.
Patch testing represents the gold standard diagnostic tool for allergic contact dermatitis. During patch testing, small amounts of suspected allergens are applied to the skin under occlusion, typically on the back, for 48 hours. The skin is then examined for allergic reactions at multiple time points. This test helps identify specific allergens responsible for the reaction, enabling targeted avoidance strategies.
For irritant contact dermatitis, the history of exposure and clinical presentation typically suffice for diagnosis, as patch testing may not be necessary. However, ruling out allergic contact dermatitis through patch testing ensures appropriate management.
Treatment Approaches for Contact Dermatitis
The foundation of contact dermatitis management centers on identifying and avoiding the causative substance. When avoidance is achieved, mild cases often resolve within a few days without additional treatment. However, when continued exposure is unavoidable or symptoms are significant, several evidence-based treatment options are available:
Topical Treatments
Corticosteroid creams and ointments represent the primary pharmacological treatment for contact dermatitis. For localized acute allergic contact dermatitis, mid- to high-potency topical steroids such as triamcinolone 0.1% or clobetasol 0.05% are highly effective. These medications reduce inflammation, swelling, and itching when applied as directed by a healthcare provider. Over-the-counter hydrocortisone cream (1%) offers a milder option suitable for mild cases and can be applied 1-2 times daily.
Emollients and moisturizers play a crucial supporting role in treatment by hydrating the skin and preventing further barrier damage. Fragrance-free, gentle moisturizers should be applied regularly, particularly after bathing, to maintain skin hydration and promote healing.
Systemic Treatments
Oral medications become necessary for severe or widespread contact dermatitis. Antihistamines such as hydroxyzine and cetirizine effectively control pruritus and reduce itching. Systemic corticosteroids are recommended for severe cases but require gradual tapering to prevent recurrence of symptoms. These oral medications work throughout the body to reduce inflammation and immune response.
Symptom Management Strategies
Beyond medications, several practical measures provide significant symptomatic relief:
- Cool compresses: Applying a cool, wet cloth to affected areas for 15-30 minutes several times daily reduces itching and inflammation
- Soothing baths: Soaking in cool water for 20 minutes with oatmeal-based bath products (such as Aveeno) calms the rash
- Avoid irritants: Discontinue use of soaps, perfumes, and dyes; use only gentle cleansers
- Protect affected areas: Avoid scratching, keep nails trimmed, and cover itchy areas with dressings if necessary
- Sun protection: Shield healing skin from sun exposure using protective clothing or sunscreen
Specialized Treatments
Calcineurin inhibitors such as tacrolimus ointment and pimecrolimus cream represent immunomodulating alternatives that inhibit calcineurin and prove particularly helpful in allergic contact dermatitis, especially on sensitive areas like the face. These agents avoid the side effects associated with prolonged topical steroid use.
Prevention Strategies
Preventing contact dermatitis involves minimizing exposure to known triggers and protecting the skin barrier:
- Personal protective equipment: Wear appropriate gloves when handling irritants or potential allergens; plastic gloves lined with cotton are ideal for frequent wet work
- Barrier creams: Apply protective creams before anticipated exposure to known irritants
- Skin hygiene: Wash hands gently after exposure, rinse thoroughly, dry completely, and apply moisturizer immediately
- Product selection: Choose fragrance-free, hypoallergenic skincare and cleaning products
- Occupational awareness: Workers should identify workplace triggers and implement appropriate protective measures
Frequently Asked Questions
Q: How long does contact dermatitis take to appear after exposure?
A: Irritant contact dermatitis typically appears within minutes of exposure, while allergic contact dermatitis may take hours or even several days to develop after initial exposure.
Q: Is contact dermatitis contagious?
A: No, contact dermatitis is not contagious. It results from direct contact with irritants or allergens and does not spread from person to person.
Q: Can over-the-counter treatments effectively treat contact dermatitis?
A: Yes, mild cases of contact dermatitis can be effectively managed with over-the-counter treatments including hydrocortisone cream, antihistamines, and moisturizers. However, severe cases require prescription medications and professional medical evaluation.
Q: How can I identify what is causing my contact dermatitis?
A: Maintain a detailed history of recent exposures, products used, and activities before symptoms appeared. For allergic contact dermatitis, patch testing by a dermatologist can definitively identify the causative allergen.
Q: Should I continue using moisturizers while treating contact dermatitis?
A: Yes, using fragrance-free moisturizers throughout the day is recommended and should be applied even on top of medicated creams to prevent skin barrier damage.
Q: What should I do if contact dermatitis becomes severe or widespread?
A: Seek professional medical evaluation from a dermatologist. Severe cases may require systemic corticosteroids, prescription-strength topical medications, or immunomodulating treatments.
Q: Can contact dermatitis become chronic?
A: Contact dermatitis is typically acute and resolves with avoidance of the triggering substance and appropriate treatment. However, continued or repeated exposure to the allergen or irritant can result in chronic dermatitis.
References
- Contact Dermatitis – Treatments, Symptoms and Prevention — Healthdirect Australia. 2024. https://www.healthdirect.gov.au/contact-dermatitis
- Contact Dermatitis: Symptoms, Causes, Types & Treatments — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/6173-contact-dermatitis
- Contact Dermatitis — National Center for Biotechnology Information (NCBI), StatPearls. 2024. https://www.ncbi.nlm.nih.gov/books/NBK459230/
- Contact Dermatitis – Treatment — National Health Service (NHS). 2024. https://www.nhs.uk/conditions/contact-dermatitis/treatment/
- Contact Dermatitis – Diagnosis and Treatment — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/contact-dermatitis/diagnosis-treatment/drc-20352748
- Diagnosis and Management of Contact Dermatitis — American Academy of Family Physicians (AAFP). 2010. https://www.aafp.org/pubs/afp/issues/2010/0801/p249.html
- Contact Dermatitis – Symptoms and Causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/contact-dermatitis/symptoms-causes/syc-20352742
Read full bio of Sneha Tete













